The Rise of Diabetes in Canada
In 2005, Sujay Nazareth, a 25-year-old IT technician in Delta, B.C., suddenly felt thirsty all the time. He began losing weight without trying, and he was tired no matter how much sleep he got. Nazareth described his issues to his doctor, who ordered a blood test. The test revealed he had type 2 diabetes. But it wasn’t a diagnosis he wanted to deal with, so he didn’t.
“I felt a lot of fear and confusion, so for the first nine years, I just hid from it,” he says. “I took my medication and tried to give up sugary things, like pop, but I wasn’t as careful as I should have been.” Nazareth also avoided doing the bloodwork his doctor routinely asked for because he was pretty sure the results wouldn’t be good. It wasn’t until his daughter was born in 2016 that he decided it was finally time to tackle his disease. “I realized that I wanted to be around for her,” he says. “It just struck me, like okay, I need to smarten up now and start taking care of myself.” He only wishes he’d started sooner.
A type 2 diabetes diagnosis means your body isn’t producing enough insulin (the hormone that controls the amount of sugar in your blood) or isn’t able to use the insulin that it produces. Too much sugar in your bloodstream puts your organs, nerves and blood vessels at risk and, left untreated, can lead to everything from heart and kidney disease to blindness and nerve damage that can result in limb amputation. Diabetes can reduce your lifespan by anywhere from five to 15 years.
Rates of the disease are rising in Canada—11.7 million of us currently have diabetes or prediabetes, largely because we’re living longer and are increasingly more sedentary. “The primary cause of type 2 diabetes is the natural aging process,” says Dr. Tom Elliott, medical director at BCDiabetes in Vancouver. “As you get older, your hair goes grey, your skin wrinkles and your cells don’t reproduce as quickly, including the beta cells that make your insulin.”
Still, a diabetes diagnosis isn’t as dire as it was even five years ago. Thanks to new treatments and technology, not to mention the promise of additional breakthroughs on the horizon, many specialists who treat the disease believe we may soon have the science to beat diabetes.
Risk Factors for Diabetes
You have a higher risk of developing diabetes before you reach senior citizen status if you are more than 40 years old, are overweight, smoke, aren’t physically active, have high blood pressure or have a family history of the disease (especially a parent or sibling). Because you can have type 2 diabetes without showing any signs or symptoms—and because making certain lifestyle changes might help prevent you from developing the disease in the first place—the Public Health Agency of Canada and the Canadian Task Force on Preventive Health Care created an online calculator where you input everything from your body mass index (BMI) to your exercise habits to help you identify your odds of becoming diabetic.
“Once you know your risk, then you can make changes, control your blood sugar levels and avoid the dreaded long-term complications that come with diabetes,” Elliott says. In addition to lifestyle changes, there are several new medications on the market that can help control weight and keep your blood sugar in check.

Symptoms of Diabetes
As with so many diseases, the sooner you discover that you’re sick, the better your treatment options will be. The most common symptoms of diabetes include increased thirst, feeling weak and tired, blurry vision, frequent urination, sudden unexplained weight loss and slow-healing sores. After following over 27,000 people for up to 11 years, Japanese researchers published a study in 2018 that found you might show early warning signs, including a high BMI and insulin resistance, up to 10 years before receiving a diabetes diagnosis—all the more reason not to skip routine checkups.
Here are 20 symptoms you should never ignore.

How to Prevent Diabetes
Almost 6 million Canadians have prediabetes, which means that your blood sugar levels are higher than normal, just not high enough to give you a full- blown diabetes diagnosis.
Not every patient with prediabetes progresses to type 2, although most will if no intervention is made, says Dr. Tamara Spaic, an endocrinologist at St. Joseph’s Health Care in London, Ontario. “We know that through diet, exercise and weight loss, you can actually prevent diabetes from developing.” Studies show that 150 minutes of exercise each week divided over five days can reduce your risk by as much as 60 per cent. Even though it isn’t easy, the fact you can have that much control over your health and change the outcome is good news, Spaic adds.
To help patients with prediabetes navigate the lifestyle changes necessary to prevent the disease from progressing further, Diabetes Canada launched the Canadian Diabetes Prevention Program. Dr. Harpreet Bajaj, director of late-phase research at LMC Healthcare in Toronto, is the study’s principal investigator and began recruiting participants three years ago to explore the effect that 12 months of one-on-one digital sessions with a personal health coach—such as a dietitian—might have on patients with prediabetes or who are at risk for type 2 diabetes (the results will be released in 2023).
The Canadian Diabetes Prevention Program is modelled after a similar initiative in the United States that led to a 58 per cent reduction in prediabetic participants developing type 2 diabetes. “We’re hoping to find something similar,” Bajaj says.
Peter Lang, a retired math teacher in Cobourg, Ontario, is one of the study’s participants. Lang, who is 74, was diagnosed with prediabetes four years ago. The program, he says, has taught him which foods to avoid—including white rice, cheese (with the exception of cottage cheese), and bananas, which get higher in sugar the more they ripen. He’s also learned how to keep his stress levels down by taking walks and getting exercise. “It hasn’t been that hard to make changes. You just get into a routine,” he says. “My wife started doing it with me. We go to the basement after breakfast to do weights for half an hour, and now I walk for about two hours a day.” Lang’s 12 months in the program are almost up, but he’s already down to his target blood sugar level—and holding.
Here’s what happens to your body when you start walking 10,000 steps a day.
Controlling Diabetes Through Lifestyle Changes
Once Nazareth decided to do something about his diabetes, he began seeing an endocrinologist. But by then, even dramatically adjusting his lifestyle wasn’t going to be enough to get his blood sugar under control. Not only did he need insulin injections, he had also developed diabetic retinopathy, caused by damage to blood vessels in the retina, that required monthly injections of corticosteroids into his eyes to prevent serious vision problems, including blindness.
Still, in addition to his medication, he worked hard at shutting down his sugar intake and increasing his physical activity. He cut down on empty carbs, like white bread, switched to Coca-Cola Zero, reduced his consumption of junk food and began walking every day. “During this time I was also diagnosed with an autoimmune condition,” he says. “And it got me thinking. I can’t control my autoimmune condition, but I can control my diabetes.”
Weight loss has always played a major role in controlling diabetes, and new research suggests it may be even more important than controlling blood sugar. Last year, an international panel of diabetes experts published a paper in The Lancet recommending that physicians shift their focus to weight first, blood sugar second. (The researchers found that dropping 15 per cent of a person’s body weight was more beneficial than lowering their glucose.)
While there are new medications that can help patients with diabetes lose weight, Canadian researchers have also been exploring how diet change might help put the disease into remission. In 2021, researchers from the University of British Columbia found that after just 12 weeks of following a meal plan of low-calorie, low-carb and high-protein foods, more than one third of the 188 participants with type 2 diabetes no longer needed medication.
“For the longest time, diabetes was considered a chronic inevitability, a disease that would progress and cause serious complications no matter what we did,” says Spaic. “Now we think we can put people into remission, akin to what is done in cancer care.”

New Drugs to Treat Diabetes
Spaic is involved in some of the latest diabetes remission research, which involves treating the disease aggressively from the outset, as opposed to the conventional approach of starting patients off with a few lifestyle changes—less sugar, more exercise, reduced stress—and waiting to see what happens to their blood sugar as a result. These so-called REMIT studies are designed to propel people with type 2 diabetes into remission.
Patients are treated with glucose-lowering medications, or the same medications combined with insulin, on top of intensive lifestyle changes, such as adopting a strict low-calorie diet. “We hope that after this intensive intervention, for at least three months, patients will have completely normal blood sugar levels without any need for medication,” Spaic says. While her own research is ongoing, other similar studies are showing a lot of promise.
Although a combination of weight loss, diet and exercise will always be at the core of diabetes care, Spaic says that some of the newer classes of drugs that have been approved by Health Canada in the last five years are having a major impact on treatment because they do more than just lower glucose. One class—called GLP 1 receptor agonists—helps with weight loss, while another—SGLT2 inhibitors—reduces the risk of heart and kidney disease.
“People with diabetes don’t die from high sugar levels. They die from cardiovascular diseases,” Spaic says, explaining that about two out of every three patients in coronary units have diabetes, while two out of five patients in dialysis units have it. “To be able to give patients a medication that will decrease their risk of heart and kidney disease by 20 to 30 per cent is huge.”
Find out how it’s possible to reverse heart disease.
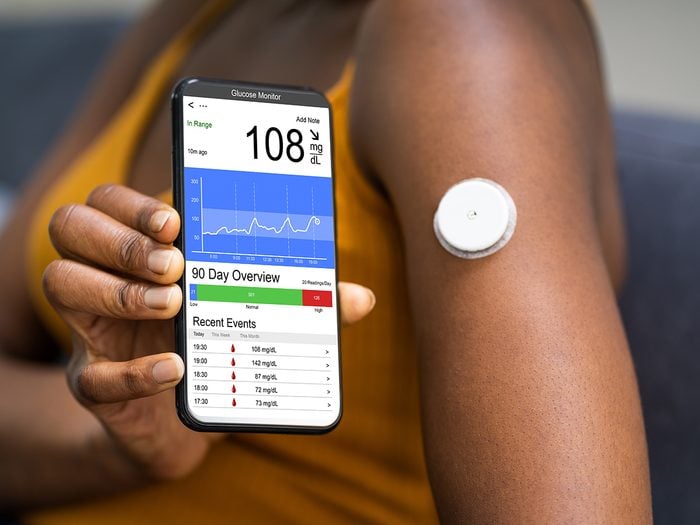
Advances in Diabetes Tech
Thanks to these new classes of diabetes medications, Nazareth no longer takes insulin and is down to a weekly injection of a GLP 1 receptor agonist that lowers his blood sugar and helps with weight control by suppressing his appetite. He also tracks his blood sugar with a continuous glucose monitor (CGM), another relatively recent development in the world of diabetes management that is still evolving.
A CGM is a small wearable device with a toonie-sized sensor attached to a tiny needle that penetrates the top layer of your skin and tests your blood sugar levels every few minutes, then sends the reading to a separate receiving device, like a smartphone.
“CGMs are something I would never have dreamed possible when I was first diagnosed,” Nazareth says. The readings let him know if he needs to adjust his medications, activity level or food intake—all in real time.
Elliott says CGMs have, thankfully, almost made the old “finger poke” method for testing blood glucose a thing of the past. CGM devices are accurate and reliable, although the sensors last only 10 to 14 days, and they are expensive. Not all provinces cover them. (Elliott successfully lobbied to get them covered by BC Pharmacare in 2021.)
“All of a sudden, you’ve got a device that tells you immediately if you made a good dietary choice. It shows you what happens if you exercise, and it shows you what happens if you get into a fight with your partner,” he says. “Just like that, we’ve got the key to the kinds of behaviour modification that each person with diabetes needs to do.”
New CGM models—smaller and even more accurate—will be arriving on the market in the next year or two, Elliott says.
Check out 10 life-saving medical innovations coming to a hospital near you.

Next Steps in the Fight Against Diabetes
It costs the Canadian health care system about $30 billion a year to treat people with diabetes, which may explain why the government invested more than $15 million in diabetes research in 2021. But all the new research into new treatments and tools won’t make a difference if diabetes patients can’t access or afford them. Laura Syron, Diabetes Canada’s president and CEO (who was diagnosed with type 2 diabetes in 2017), pushed for a Canada-wide framework in a bill that was made law last year.
“We have a national strategy for cancer and one for mental health, but we didn’t have one for diabetes.” The framework will help turn the patchwork of programs across the country into a single unified network that can share information and best practices when it comes to everything from prevention and quality of care for patients to ensuring Canadians get equal access to the latest treatments.
Next, her goal is to change the conversation around the disease. Syron is tired of how diabetes is portrayed in the media, and that when the disease is mentioned in a newscast, the camera inevitably cuts to a shot of an overweight person eating ice cream. There is a persistent, misguided perception that if you have diabetes, it’s your fault, she says. Syron would like to see greater compassion for people with the disease and more widespread understanding that there are multiple factors that cause it.
“When I was diagnosed, I felt like I’d failed, like I’d eaten too many french fries,” Syron says. “I stigmatized myself.” Over the years, reactions to her disease have ranged from apathy (“You’re lucky it’s not something worse”) to blame (“You brought this on yourself”).
“It’s an exhausting disease, a constant worry where you can never stop monitoring yourself,” Syron says. “But just 100 years ago, a diabetes diagnosis was a death sentence. When insulin was discovered, it was a huge leap forward, but since then we’ve seen only incremental changes—until now.”
Lately it seems as though every month a new diabetes study is released, many of them Canadian. In January, a new clinical trial from researchers at the University of Alberta found that insulin-producing cells grown from stem cells can be safely implanted into the abdominal wall of a patient with diabetes. It was a small trial, but 35 per cent of the patients who received the credit card–sized implants showed signs of insulin production in their blood within six months of the implant, and 63 per cent showed signs of insulin production a year later.
All of this momentum, from investment to research, gives diabetes doctors hope that someday there will be a cure. “That’s something that we have to continue to strive for,” Spaic says. “Every generation likes to say we will have one in 10 to 15 years, but considering how today’s diabetes research is expanding our understanding so exponentially, I’m sure that cure will come.”
Now that you know how to prevent diabetes, learn how to spot the heart attack symptoms that are frequently misdiagnosed.