How Stem Cell Therapy is Saving Lives
New medical advances promise relief from back pain, vision loss, multiple sclerosis, osteoarthritis and other diseases—all using stem cells, the building blocks of our own bodies.

Breakthroughs in Stem Cell Therapy For Back Pain
Annissa Jobb had been working as a personal support worker in Toronto for a couple years when her back pain first appeared. The cause: an undiagnosed herniated disc, which had pinched the nerve. As the pain worsened, she gritted her teeth and tried to keep going.
“It was my calling in life, taking care of people,” explains Jobb, now 54. But working with frail seniors involves a lot of lifting, bending and pulling. “I had a drawer full of pain medication. None of it was working. I’d snap. My husband and I came close to getting divorced.”
By November 2016, about a decade after she first noticed the pain, Jobb could scarcely walk 200 metres. “My family doctor finally said, ‘You will end up in a wheelchair if you don’t stop working there.’”
Jobb’s GP referred her to Dr. Riam Shammaa, a sports medicine and pain specialist in Toronto. Every few weeks, Shammaa administered nerve-block needles, similar to an epidural. They held Jobb’s pain at bay for anywhere from a few days to a few weeks, but then it always returned.
Historically, the treatment of chronic back pain has been less than ideal, either causing patients to become addicted to opioids or involving major—often unsuccessful—spinal-fusion surgery, which is suitable for only about one in 20 patients. Hunting for a solution beyond these limited options, Shammaa turned to stem cells—the building-block cells found in human embryos, but also in various tissues in adult bodies—which are able to generate an array of different cells. Specifically, he’d been studying bone marrow stem cells, and invited Jobb to participate in a study with 23 other patients, cautioning that there were no guarantees. The procedure would involve using Jobb’s own bone marrow cells and had been proven safe. She agreed to try it.
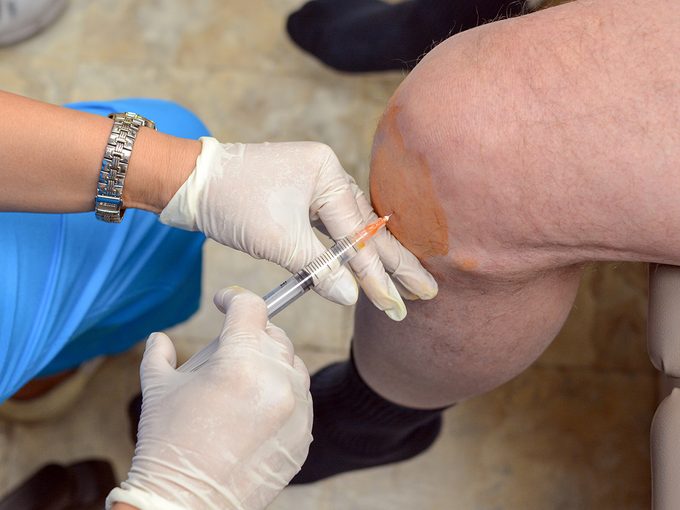
In Jobb’s case, the stem-cell therapy would require extracting her bone marrow tissue and concentrating the stem cells, known as mesenchymal stem cells, or MSCs, present in the marrow. This concentrate (called bone marrow aspirate concentrate, or BMAC), which is processed in a centrifuge, would then be injected into her herniated disc in the hopes that it would regenerate and heal the damaged tissue.
An MRI of Jobb’s spine showed two discs were causing her problem, which was good news as far as the procedure was concerned. “Out of five levels on the lumbar spine, one or two showing damage tells you that the spine hasn’t deteriorated everywhere,” says Shammaa. “By contrast, when you have five levels of severe disc disease—in other words, if the spine is really messed up—there is not a lot you can do.”
The procedure took place in September 2017 and began with an extraction of Jobb’s bone marrow—the most painful step—which was immediately distilled and concentrated. Then, guided by a type of X-ray called fluoroscopy, Shammaa inserted a needle through Jobb’s spine to place the BMAC in the discs. All told, it took three and a half hours, and Jobb remained awake the entire time in order to alert Shammaa if he touched a nerve.
Afterwards, Jobb recovered in bed for two weeks and then, slowly, began to walk. A month later, however, she strode briskly into the clinic, a moment Shammaa recalls with delight. “She was in disbelief,” he says.
When Shammaa published his findings in March 2021, he reported that 90 per cent of his patients gained two to three millimetres of height that had been lost due to disc compression. Furthermore, 80 per cent of them stopped using opioids. As for Jobb, while she had previously described her back pain as “beyond 10,” she says it’s now a two.

The Regenerative Medicine Revolution
The use of stem cells is part of a field called regenerative medicine, which began to emerge two decades ago as a way to deploy the body’s own cells and growth factors to repair tissues by restoring their lost function. Several such therapies and products are already approved by regulators and in use, including skin substitutes for treating burns, scaffold products for healing surgical incisions and cord blood-derived products for treating certain blood diseases and disorders.
But over the next decade, the expanded use of stem cells to treat even more injuries and conditions could lead to a medical revolution. As researchers report from stem-cell clinical trials being conducted all over the world, the hope that these cells can repair damaged bodies, long discussed and debated in scientific circles, appears to be well founded.
In a study treating congenital vision loss with retinal stem cells at the University of California, Irvine, for instance, one woman was able to see her family for the first time in years. A German child suffering from a sometimes-fatal skin disease called epidermolysis-bullosa recovered after receiving a transplant of genetically modified skin cells at Italy’s University of Modena and Reggio Emilia. The actor Selma Blair reported symptom remission last August after participating in a stem-cell transplant trial for multiple sclerosis. And a multi-centre study on treating osteoarthritis underway in Ireland, France and the Netherlands shows promising early results from 18 patients.
Despite these early successes, Shammaa cautions that the science is so new that it is easily misunderstood and misapplied. “There are a lot of snake-oil salesmen out there,” he says, pointing to private stem-cell clinics all over the world that claim to cure such things as erectile dysfunction and dementia, doing so without genuine evidence and in defiance of regulatory bodies. “It’s important for patients to learn what is possible right now and what is still down the road.”
He adds, “Some patients are good candidates for simple procedures like a bone marrow concentrate injection, but others have illness or injury that is too advanced or too complicated. We cannot give them false hope.”
That said, the field of stem-cell therapy is less than 20 years old and has already come a long way.
The Future of Stem Cell Therapy
An early breakthrough occurred in 2006, when Shinya Yamanaka, a molecular biologist at Kyoto University in Japan, showed that stem-cell therapy could avoid the morally divisive use of embryonic stem cells. Instead, he discovered he could induce adult skin cells to develop into blood or bone or liver cells. Yamanaka, who went on to win the 2012 Nobel Prize for this work, differentiated these cells from the kind found in a fertilized egg by calling them “induced pluripotent stem cells,” or iPSCs. While an embryo’s “totipotent” cells could turn into any part of the body, iPSCs could create many different kinds of tissues, but not a whole human. Since this discovery moved the conversation about stem cells past the sensitive subject of using fetal tissue for medical purposes, which is illegal in some countries, the research began to take off.
In 2014, Tokyo’s Riken research institute performed the first-ever successful iPSC transplant, creating retinal cells generated from skin cells from a patient with age-related macular degeneration. Shortly afterwards, Dr. Henry Klassen at the University of California, Irvine, oversaw a trial for treating retinitis pigmentosa, a rare genetic group of disorders causing gradual blindness, in which a donor’s retinal progenitor cells were transplanted into the eyes of 28 study participants. One of them, 64-year-old Kristin Macdonald of Los Angeles, who had gone blind, regained what she describes as a burst of light. “I can navigate by light now, and see more contrasts and shapes,” she says. Macdonald has since become an outspoken patient advocate for stem-cell trials.
Then, in 2018, neurosurgeon Richard Fessler of Rush University Medical Center in Chicago oversaw a year-long trial with iPSC stem cell-derived motor neurons transplanted into six patients paralyzed by spinal cord injuries. Fessler reported that all regained some upper-body movement, and that a patient who was only able to shrug his shoulders can now use his hands to eat, write and do other tasks. This is the kind of breakthrough that the late Superman actor Christopher Reeve was advocating for from his wheelchair, after neck-down paralysis from a horseback-riding accident, while governments around the world were making moves to restrict embryonic stem-cell research. (In certain cases, embryonic stem cells are in medical use, derived from leftover blastocysts—the clustering of cells in a fertilized egg—that didn’t implant during an IVF treatment.)
These are still early days, with much to investigate in terms of safety, dosing and how to manufacture iPSCs for different conditions in a standardized and cost-effective way. But Yamanaka predicted in 2018 that several treatments using regenerative medicine and new drugs will be developed, authorized and covered by insurance as soon as 2030.
“We’re looking at regenerative medicine as something that will one day be a medical specialty of its own,” adds Dr. Shane Shapiro, associate professor of orthopedic surgery at Mayo Clinic in Jacksonville, Florida, “much like cardiology or neurology.”
In the meantime, the first generation of stem-cell treatments that currently have regulatory approval in Canada, the U.S. and the European Union largely involve simple cell transplants—ones that move the patient’s own cells from one part of their body to another. That said, stem-cell transplants for blood diseases like leukemia have been used for several years, this being the one exception where a matching donor’s cells are also allowed.
Among approved procedures, the most common is BMAC transferred to the spine or the knee. While Jobb sought treatment for her back, 58-year-old telecommunications technician Rodolfo Corsini was looking for relief for job-related knee pain when he visited Italy’s Humanitis research hospital in 2020. He had never heard of BMAC until it was suggested to him by surgeon Elizaveta Kon, who didn’t see enough damage to merit knee replacement surgery. He agreed to the injection, and it was a success. “I can do almost everything that I did before,” he says.
Kon, along with some European colleagues, is now involved in a number of exploratory studies, including a comparison of treating patients with BMAC plus another type of adult stem cell—called stromal vascular fraction (SVF)—which is extracted from a person’s fat tissue.
Will it work? Certainly the early research on BMAC provides hope, although with limitations. “We couch these treatments as something to help with a chronic, degenerative condition, something that in many cases can be successful in managing the symptoms and improving quality of life but in most cases are not a cure,” Shapiro says. “The analogy should be diabetes or high cholesterol. We don’t cure those things; we treat them. What we would like to see in the future is a way to treat arthritis without metal and plastic, or to treat degenerative disc disease without a spinal fusion. That’s the ultimate goal.”
A consortium of 10 European partners, including universities, is in pursuit of that goal, and researchers are even looking to skip the painful marrow extraction procedure that Jobb underwent. Instead, says research scientist Mary Murphy at National University of Ireland, Galway, they hope to be able to create MSC cells in the laboratory in a standardized and high-volume way. And while some members of the EU-funded group are focusing on how to generate that sustainable supply, others are testing new therapies. For example, researchers in Sweden and the Netherlands are currently developing one for osteoarthritis. It will be several more years before everything can be tested, approved and made available.
Because regenerative medicine is still young, and patients should be wary of profit-hungry companies selling fraudulent stem-cell products, those who want to know their options should start by consulting with a medical expert on their specific condition. “If it’s knee arthritis, start with a specialist in orthopedic surgery or sports medicine,” advises Shapiro. “If it’s degenerative disc disease of the lumbar spine, start with a spine specialist.” Then, seek a referral to someone in that field who has learned about regenerative medicine.
For many patients, stem-cell therapy is already making a lasting difference to their quality of life. “My husband and I went hiking last summer,” Jobb says. “I walked a whole kilometre. I was so excited. I thought, maybe I could start cross-country skiing! Why not?”
Types of Stem Cells
Here are the main types of stem cells being used in the rapidly developing field of regenerative medicine.
By Tina Knezevic
Pluripotent
A few days after fertilization, an embryo becomes a mass of about 100 cells (a blastocyst) that can become any type of body cell. Since there are ethical concerns with harvesting them, scientists are learning to reprogram adult cells to act like pluripotent stem cells. These induced pluripotent stem cells (iPSCs) hold promise for diseases like macular degeneration, Parkinson’s and heart disease. (Don’t miss these tips on how to reverse heart disease.)
Multipotent
Multipotent stem cells can develop into more than one cell type but are more limited than pluripotent cells. For instance, mesenchymal stem cells are a type of multipotent cell that can come from bone marrow, fat tissue (from stromal vascular fractions), an umbilical cord or amniotic fluid. They’re popular in regenerative medicine, and there’s potential for them to treat many conditions, including spinal cord and cartilage injury, as well as rheumatoid arthritis.
Unipotent
Unipotent stem cells can become only one thing. There is research underway to see how skin stem cells could be used to regenerate skin after burns, which would normally be treated with skin grafts.
Next, put your knowledge of medical trivia to the test.






