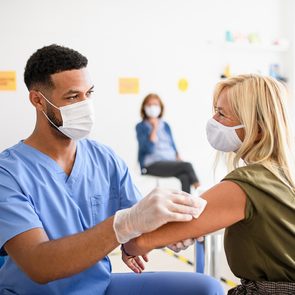
What You Need to Know About Blood Clots and COVID-19 Vaccines
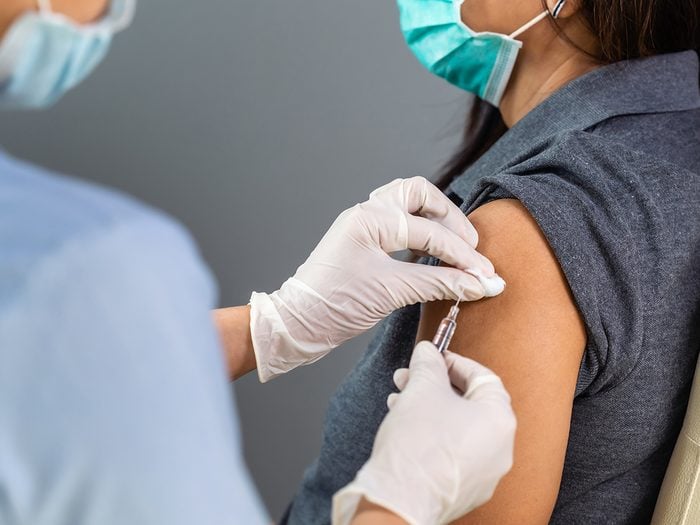
Concerned about the risk of blood clots associated with the AstraZeneca COVID-19 vaccine? Canadian medical experts shed light on the science behind this rare (but serious) reaction.
It’s been a while since blood clots last made the news. In the mid-’90s, doctors raised the alarm about a connection between blood clots and oral contraception. Known as The Pill Scare, reports that new higher-dose formulations of oral contraception increased the risk of venous thromboembolism (VTE) prompted many women to switch brands or stop using oral contraception all together.
Recently, blood clots are back in the headlines because of reports of a very small number of cases associated with the AstraZeneca and Johnson & Johnson vaccines for COVID-19.
What are blood clots?
Far from being a bad thing, clotting is one of the body’s natural, life-saving processes.
“Your body intrinsically has a clotting system and a blood thinning system, and they work in balance,” explains Dr. James Douketis, Professor of Medicine and Chair in Thromboembolic Disease at McMaster University in Hamilton, Ont.
Cut your finger on a piece of glass and your body kicks into clot mode to stop the bleeding. Tiny blood cells called platelets rush to the scene and begin to stick together. A chemical reaction is then initiated in which a clot is formed, and the process of repair begins. Eventually, a reverse chemical process occurs to dissolve the clot. Normally, a blood clot will dissolve on its own.
When the body’s natural clotting and blood thinning system is out of balance, however, you bleed when you shouldn’t or form blood clots when you shouldn’t—and that can be a problem.
How do you get a dangerous blood clot?
Three factors can influence the development of a blood clot, says Douketis. They are injury to a blood vessel, poor blood circulation or biochemical changes to the blood that predispose you to clotting.
Cancer, recent surgery or an existing medical condition are all factors that are associated with elevated risk of developing a blood clot. Pregnancy heightens the risk for blood clots for women as does the use of oral contraceptives, to about five times more than normal and between two to four times more, respectively. (Contraceptive patches and rings also have elevated risks.)
With age comes a greater risk of developing a blood clot. About one in 1,000 adults over the age of 45 will develop a blood clot each year, says Douketis. For younger people, the risk is lower and hovers around one in 10,000 each year.
The most common spot to get a blood clot is in the legs, which is known as deep vein thromboembolism (DVT). DVT has the potential to see particles from that clot travel through the bloodstream to the blood vessels in the lungs and create a blockage (known as pulmonary embolism), a far more serious clot.
Clots can also cause heart attacks and strokes.
“The way most heart attacks start is that you have a fatty deposit in the wall of an artery, [part of] that fatty deposit cracks and the body thinks, ‘Oh, there’s a cut! I’d better clot.’ It forms a clot, blocks the artery and you have a heart attack,” explains Dr. Harry Rakowski, a cardiologist at the Peter Munk Cardiac Centre in Toronto.
A blood clot that causes heart attack or stroke can develop over a period of years, whereas a blood clot in the venous system of the leg or groin can spring up suddenly over a period of days.
How do you treat blood clots?
How you get a blood clot—what Douketis calls the “disease process” of the clot—can affect how it is treated.
For example, aspirin is sometimes used as a treatment for clots related to heart attack and stroke. Other clots may be treated with anti-coagulant drugs (a.k.a. blood thinners).
What’s different about the blood clots associated with the AstraZeneca vaccine from other types of blood clots?
The blood clots associated with the AstraZeneca vaccine are known as vaccine-induced immune thrombotic thrombocytopenia (VITT). The main difference between these blood clots and “garden variety” blood clots, says Douketis, is the way they develop.
These clots are not linked to traditional risk factors but appear to be the result of a rare but abnormal immune response to one component of the vaccine’s adenovirus vector or immune response trigger, explains Douketis.
The AstraZeneca vaccine uses a weakened version of a common cold virus (adenovirus) that contains the genetic material of the now-familiar SARS-CoV-2 virus spike protein to prime the immune system to fight the virus.
It’s the same technology used in the Johnson & Johnson vaccine, which has also been associated with a small number of rare blood clot reactions. (The U.S. resumed use of the Johnson & Johnson vaccine in late April after 15 reported cases of blood clots occurred out of eight million doses administered. On May 3, Canada’s National Advisory Committee on Immunization (NACI) deemed the vaccine safe for use in people 30 and over if they can’t wait for mRNA COVID-19 vaccines, which NACI admits to preferentially preferring.)
It’s not clear what component of the vaccine’s vector causes VITT, but the reaction is essentially an abnormal immune response that activates the platelets, the tiny blood cells that help the body form clots, that then sets off a dramatic clotting response within the body. Clots can form in the veins and arteries, and even the brain.
Rakowksi likens this “idiosyncratic” reaction to a similar drug-induced clotting condition known as heparin-induced thrombocytopenia (HIT). (Heparin is an anti-coagulant, and in around 5 per cent of patients taking it, it triggers a similar adverse clotting response in the body.)
The kind of clotting associated with this adverse reaction, however, can be more serious because it can cause clots to form in many places and can cause a cerebral venous sinus thrombosis (CSVT), or brain clot.
What’s the risk of getting a blood clot with the AstraZeneca vaccine for COVID-19?
While the clots can be serious, the incidents of these complications are rare and occur in approximately 1 in 100,000 people, according to the European Medicines Agency, which paused use of the vaccine to investigate adverse reaction reports in early March (the agency deemed the vaccine safe, arguing its benefits to all age groups outweighed its small risk to VITT shortly after).
As of April 29, more than 2.3 million doses of AstraZeneca have been administered in Canada. In total, only seven cases of blood clots have been reported. In Ontario, there have been three reported cases among over 700,000 vaccinations; in Quebec, where more than 500,000 AstraZeneca vaccines have been administered, there have been three cases reported by the province’s health ministry. Of the three, one was fatal.
What is the treatment for VITT?
The unique process by which the clots develop, however, means that treatment needs to be specific, too. Douketis speculates that the high rates of mortality related to this reaction in Europe where the vaccine was initially given, may have had a lot to do with evolving understanding of the reaction itself. Doctors may have assumed the clots could be treated with blood thinners immediately, an unintentional error that may have accelerated the clotting process.
“This is a very unusual type of blood clot and has to be treated in a very different way,” he explains.
The current thinking is that before the clots can be treated, the hyperactive immune response needs to be dealt with.
“The frontline treatment is anti-immune medications to suppress or put down the fire and the blood thinners clean things up, in a manner of speaking, by helping the body melt away the existing blood clots.”
The necessity of specific intervention makes awareness of the symptoms of VITT vital. This rare but serious reaction tends to occur within four to 30 days of vaccination and can include:
- Severe headache
- Visual changes
- Abdominal pain
- Leg pain or swelling
- Easy bruising or bleeding
- Nausea and vomiting
- Back pain
- Shortness of breath
Should those symptoms present themselves and linger after the normal 24- to 48-hour window associated with regular vaccination reactions such as fever or muscle aches, immediate medical attention is advised.
Rakowski points out that a blood test to determine platelet count taken five to seven days after vaccination could help identify VITT, though it may not be a cost-effective approach given the small risk of developing clots.
The nature of the rare adverse reaction means most people, even if they have a history of blood clots, do not have increased risk of blood clot if they take the AZ vaccine. (People who have a history of brain clots, however, are advised to take another vaccine.)
How should Canadians weigh the risks and benefits of the AstraZeneca vaccine?
The risk of hospitalization and death from COVID-19 currently outweigh the comparatively minimal risk of experiencing a rare adverse event due to vaccination. As Douketis points out, COVID-19 itself presents a heightened risk for developing serious blood clots in the lungs.
More than 24,000 Canadians have died from COVID-19 since the pandemic began. While age is associated with an increased risk for the most serious outcomes, rates of severe illness have increased in the third wave, particularly among those aged 40 to 59, while those aged 20 to 39 account for highest cases overall.
In addition to potentially reducing transmission rates, vaccination appears to confer some protection against developing the more serious complications that can result from COVID-19 infection.
Risk-to-reward ratios are at the centre of every public health measure, from speed limits to oral contraception. They also form a fairly common personal basis for decisions that individuals make on a daily basis, says Rakowski. While concerns around vaccines should not be dismissed, he says those concerns should be vetted within the context of the pressing and significant threat of COVID-19.
“Take the first vaccine offered to you because the benefits outweigh the risk right now,” says Rakowski.
Next, find out what you can (and can’t) do after getting your first dose of the COVID-19 vaccine.