
If it wasn’t a urinary tract infection, what was it?
The patient: Samantha (name has been changed), a 24-year-old waitress
The symptoms: Lower back pain and exhaustion
The doctor: Dr. Andrew Rule, nephrologist at the Mayo Clinic Hospital, Rochester, Minnesota
Samantha, a waitress who spent most of her days on her feet, hardly ever got sick. But in October 2017, she started feeling rotten. She was tired all the time and began to wonder if she had the flu. At the restaurant, she just wanted to crawl under a table. Her regulars could tell something was wrong.
During this period, Samantha also felt an intermittent, stabbing pain on the right side of her lower back. She noticed her urine looked cloudy, which made her suspect a urinary tract infection—or, worst case, a kidney stone.
When nothing resolved after two weeks, Samantha visited her family doctor, who checked her urine. She was negative for a UTI, so the doctor took some blood and sent Samantha for a CT scan of her kidneys.
The next day, the doctor called to tell her there was no kidney stone, but that Samantha’s level of creatinine, a waste product, was rising. Also, her urine contained blood and protein. Unable to explain it, Samantha’s doctor referred her to the Mayo Clinic’s emergency department.

A rare diagnosis
Nephrologist Andrew Rule ascertained from additional blood tests that Samantha’s kidneys were losing function rapidly; he guessed that something could be causing inflammation of her glomeruli, networks of tiny blood vessels in the kidneys that help filter waste. Rule ordered new tests to look for possible causes, such as lupus, and gave Samantha a high-dose steroid to control inflammation. “Time is critical for kidneys,” he says. “If they stop working, they may not come back.”
Rule discovered that Samantha’s blood contained antibodies, created by her own immune system, that were attacking the glomeruli. When this happens, these clusters of fragile blood vessels in the organ break down and bleed. If the problem isn’t treated soon enough, patients not only lose their kidney function—they can lose their lives.
The rare condition, known as anti-GBM disease (named after the antibodies), occurs most often in people who are in their 20s or over 60. Doctors remain in the dark about the reason for this age split, and about some other aspects of the disease. “It’s not known what triggers these antibodies to be produced in the first place,” says Rule.
Learn how to spot the silent signs of lupus.
The treatment begins
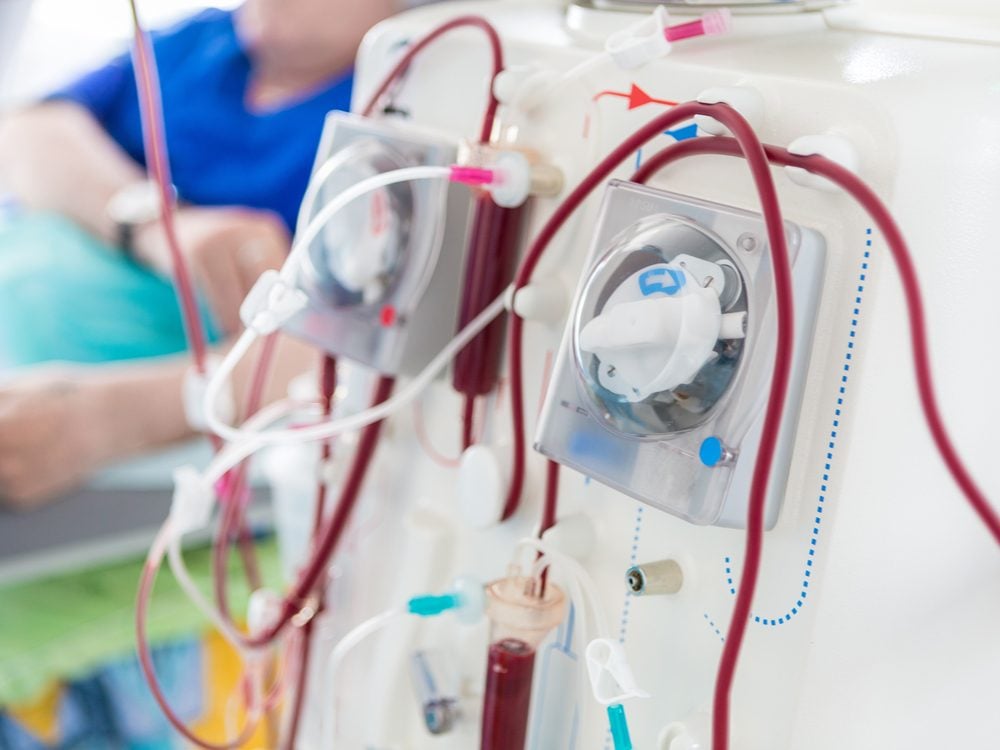
Treatment, which must begin right away, includes steroids, chemotherapy and sometimes rituximab, an antibody therapy. On top of this, Samantha’s blood would be removed each day to filter out the plasma with the damaging antibodies, and then returned to her veins along with donor plasma.
After seven days of this regimen, Samantha’s creatinine levels hadn’t normalized, so she began dialysis—three sessions a week—to do the work of her impaired kidneys.
Eighteen days later, the antibodies had lowered enough for her to go home. She would continue dialysis but eventually, doctors told her, she would need a kidney transplant.
Read the powerful story of how one woman’s kidney donation saved her cousin’s life.

A miraculous recovery
Then, a couple days before Christmas, she got wonderful news that came as a complete surprise: not only was the treatment performing well, and the antibodies’ assault on her kidneys easing up, but some function had resumed. “None of us expected that,” says Rule, explaining that while many of Samantha’s glomeruli were damaged beyond repair, others had must have started working extra hard. She no longer needed dialysis, let alone the transplant.
Today, Samantha is back at work. Although her kidneys will never be completely normal, she does her best to keep them healthy by watching her intake of salt and potassium.
“I had about 40 people offering me their kidneys,” she says. “But I didn’t want theirs—I just wanted mine.”
Next, check out 20 symptoms you should never ignore.