
1. Overweight? I May Not Bring it Up
When people are massively overweight, it’s an obvious issue. When they’re only moderately overweight, it’s harder to bring it up, because society accepts people being a little overweight. It’s harder to tell someone like that they have weight to lose. –Stuart Connolly, MD, director, division of cardiology at McMaster University in Hamilton, Ontario
(Photo: Wavebreak Media/Thinkstock)

2. Sugar, not Fat is the Real Problem
When you eat refined sugar, you create an insulin response that is toxic to blood vessel linings. Most attention seems to be on cholesterol; I don’t know that doctors are checking insulin and A1C levels [measures of diabetes risk, which is closely linked to heart health]. –Stephen Sinatra, MD, cardiologist and author of numerous books about heart health, including The Great Cholesterol Myth
(Photo: iStockphoto/Thinkstock)

3. Most Supplements are Ineffective
Doctors who strongly recommend certain supplements are often the ones selling them in their office. For primary prevention, if you’re not eating fish two to three times a week, then fish oil is probably a good idea. I also recommend vitamin D because 80 percent of U.S. adults are deficient. Those are the only two I take. –Sarah Samaan, MD, cardiologist at The Legacy Heart Center in Plano, Texas and author of Best Practices for a Healthy Heart
(Photo: iStockphoto/Thinkstock)

4. I Need to Know if You or Your Partner Aren’t Sleeping Well
Sleep apnea is a major cause of cardiac events such as heart attack, cardiac arrest, and stroke. If you suspect you have sleep apnea (snoring and feeling exhausted when you wake up are big clues), you should tell your doctor about it. If your spouse is always nagging you for snoring, that’s an important sign too. –Stephen Sinatra, MD, cardiologist
(Photo: Stockbyte/Thinkstock)

5. Had a Dramatic Pregnancy? Tell Me
Preeclampsia is a hidden risk factor for early heart disease. It tells me that there’s an underlying problem with the blood vessels. Young women should recognize it’s important for their doctor to know if they develop it. And most doctors won’t ask a 50-year-old woman about her pregnancy health from 25 years ago.The same goes for rheumatoid arthritis and lupus. Heart attacks are the number one cause of death in these patients, and they need aggressive management of risk factors. -Malissa J. Wood, MD, co-director of the Women’s Heart Program at Massachusetts General Hospital
(Photo: iStockphoto/Thinkstock)

6. Red Wine isn’t a Cure-all
My patients tell me, “I started drinking red wine” and I say “what for?” They think its good for the heart, but you have to be careful not to overdo it and raise your risk of other health issues. Same goes for dark chocolate. People think that you can eat as much as you want. It is good for you-it lowers blood pressure and has antioxidants-but most people are not eating just that one ounce a day. –Stephen Sinatra, MD, cardiologist
(Photo: iStockphoto/Thinkstock)

7. What Makes Me Mad? Smoking
If someone’s a smoker, they gotta stop. I feel sick when I talk to people who still smoke. It’s never too late to stop. Even quitting in your seventies improves survival. If patients want to do one thing for their health, it should be to stop smoking. -Stuart Connolly, MD, director, division of cardiology at McMaster University in Hamilton, Ontario
(Photo: Wavebreak Media/Thinkstock)

8. A Prescription is an Easier Solution, but Not Always a Better One
Emotional toxicity is a major cause of heart disease. Depression, heartbreak, and uncontrolled anger are major risk factors. A good cardiologist can see that a patient is suffering from these issues. Many doctors believe in drugs but less in healing the whole person. –Stephen Sinatra, MD, cardiologist
(Photo: Comstock/Thinkstock)

9. I Should Examine Your Teeth
If you have lots of inflammation in your mouth, it’s a sign your whole body is experiencing an inflammatory response. Patients with gum disease have much more heart disease. I always check my patients’ mouths. –Stephen Sinatra, MD, cardiologist and author
(Photo: iStockphoto/Thinkstock)

10. Your Family History Isn’t as Bad as You Think
People will come in and say “my grandma died of a heart attack when she was 80, so heart disease runs in my family.” That’s not true-everyone has to die of something. We define family history as a cardiac event before age 60 in women and before 50 in men. It’s far narrower than people realize. –Sarah Samaan, MD, cardiologist
(Photo: Digital Vision/Thinkstock)
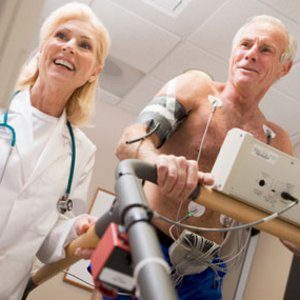
11. You Probably Don’t Need that Stress Test
People used to start getting them at age 50 and then get them yearly. But a stress test will only pick up blockages of 70 per cent or greater. A normal test doesn’t mean you don’t have blockages. There’s no medical reason to have a stress test unless you have symptoms, like chest pain or shortness of breath, or an abnormal EKG. –Sarah Samaan, MD, cardiologist
(Photo: iStockphoto/Thinkstock)
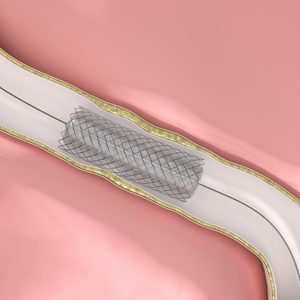
12. That Stent Might Not be Necessary
If a blockage is not causing symptoms or a reduction in blood flow, then it doesn’t need to be stented. In the absence of a severe blockage, treating with medication is just as good. And once you do a stent, then you need to do another, and the problem can proliferate. –Malissa J. Wood, MD
(Photo: iStockphoto/Thinkstock)

13. I Want to Hear Questions, from You or your Family
The best time to get my attention is the first few minutes of the appointment, before I start the physical exam. That’s when you need to bring up the things that are bothering you. I also like when you have a family member or friend to help. You may be hearing hard news and walk away with mixed messages. –Malissa J. Wood, MD
(Photo: Photos.com/Thinkstock)

14. Your Blood Pressure at Home Matters More than at Work
I see a lot of white-coat hypertension [where blood pressure is elevated in the office but normal at home]. If patients are surprised by their blood pressure number, I’ll retest it or ask them to record it at home for a week and bring in their readings. This way if it is high, they’re more motivated to work to lower it. –Sarah Samaan, MD, cardiologist
(Photo: iStockphoto/Thinkstock)

15. Tell me the Truth: Do You Suffer from Erectile Dysfunction?
Erectile dysfunction is also marker of blood vessel disease. The small blood vessels are a barometer of what goes on in the large blood vessels. My own father found out that he had a blockage in his neck when he went in for a prescription for [ED]. –Malissa J. Wood, MD
(Photo: iStockphoto/Thinkstock)