
Coping with seasonal allergies
Call them seasonal allergies, hay fever, pollinosis or allergic rhinitis. But don’t dismiss them as “the sniffles” to the millions of people worldwide whose quality of life takes a dive at particular times of the year. Sneezing and a runny nose may be the most obvious symptoms, but pollen allergies can also trigger itchy eyes, a sore throat, coughing, headaches, fatigue, skin rashes and, if left untreated, even asthma attacks. Although seasonal allergies usually begin in childhood, they can develop during any stage of life. Experts warn that climate change may bring a rise in pollen levels and a corresponding increase in misery in the coming years, so here are some strategies to help you cope.

1. Pay attention to the pollen report
To start, check your local pollen reports and plan activities accordingly. Generally, right after a downpour is the best time to venture outdoors, because the rain drags airborne particles to the ground. If you must do yardwork, wear a protective mask.
Find out why meteorologists get forecasts wrong.

2. Make your home a sanctuary
Until pollination time passes, keep your doors and windows shut as much as possible. (Allergy seasons vary by region: in temperate climates, they’re generally in springtime for tree-allergy sufferers, May through July for those allergic to grass pollens and late summer to early autumn for those set off by ragweed or mugwort.)
Be sure to never miss these spots when spring cleaning.

3. Don’t bring the outdoors in
After a stint outdoors, change your clothes and take a shower to remove pollen from your skin and hair. High-efficiency particulate air (HEPA) filters, designed to capture 99.97 per cent of airborne particles, should snag the sneakiest of allergens.
Find out if Ikea’s new air purifier is worth it—and if it works.
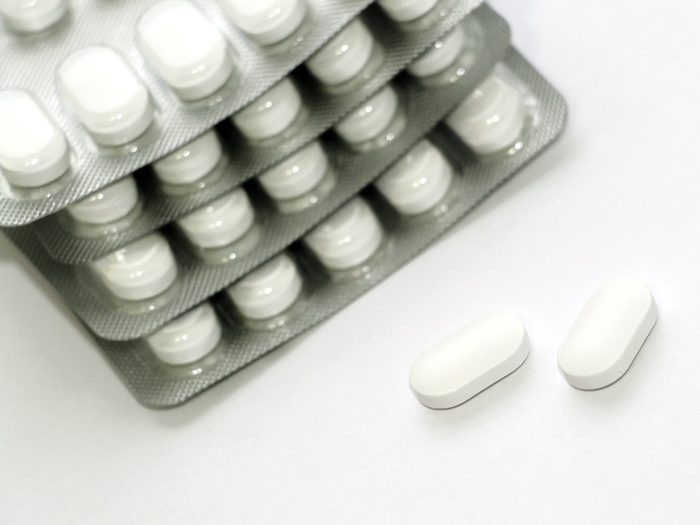
4. Combat seasonal allergies with antihistamines
If avoiding triggers isn’t realistic, there are drugs at your disposal. In the over-the-counter category, antihistamines can be taken even before symptoms start on high-pollen-count days. Corticosteroids, which require a prescription, pack an even greater punch.
Don’t forget to ask your pharmacist these important questions when picking up a new prescription.
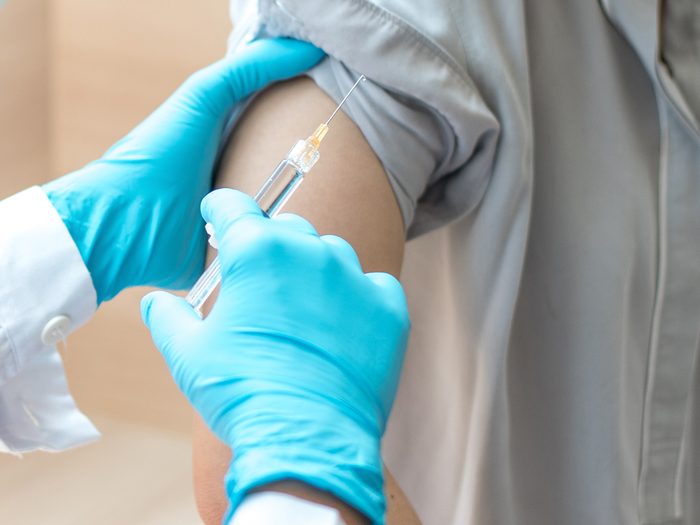
5. Consider immunotherapy
There’s also allergen immunotherapy (AIT): injections, tablets or drops that expose you to ever-larger doses of your trigger substance. While they do require regular doctor visits for months or even years, “their beneficial effects are sustained for years after the treatment course has ended,” explains Dr. Oliver Pfaar, head of the rhinology and allergy department at University Hospital in Marburg, Germany. AIT also helps prevent new or more severe allergies, Pfaar says, because it attacks the root cause of symptoms: an immune system that sees harmless particles as intruders.
Next, find out what triggers might be causing adult-onset allergies.