New hope for aging knees
A power drill whirs noisily—shavings curl from the bit as it bores a precise hole. Cement oozes from a caulking gun to join two surfaces. A hammer whacks repeatedly on metal. Behind the workers, a busy crew shares measurements and part sizes.
It’s the sounds of renovation, but it’s not a new kitchen. In a hospital in Philadelphia, a medical team led by orthopedic surgeon Dr. Matthew Austin is replacing a knee joint. It is his fifth surgery of the day. An hour later, he’s off to his next case while the rest of the team handles the final details.
Three hours after the surgery wraps up, Ralph Gabriel, then 69, the construction business owner upon whom those tools whirred and banged, is awake and joking with his family. He didn’t want surgery. But years of tile installation had destroyed the cushion of cartilage in his right knee, creating constant pain from bone grinding on bone. ”You have to have the will to get it done,” Gabriel says.
These are the serious health symptoms you should never ignore.

Lessening the pain
The human knee is particularly vulnerable to wear. Every step, every jump, every crossing of the legs, puts stress on the joint. When you combine the active lifestyle of the over-50 population and longer life spans, it’s no wonder that an increasing number of people are experiencing knee pain.
There are many short-term remedies, says Dr. Nortin M. Hadler, who is such as weight loss, physical therapy, knee braces, injections and supplements, but for a perpetually painful or arthritic knee, the go-to solution is to replace it.
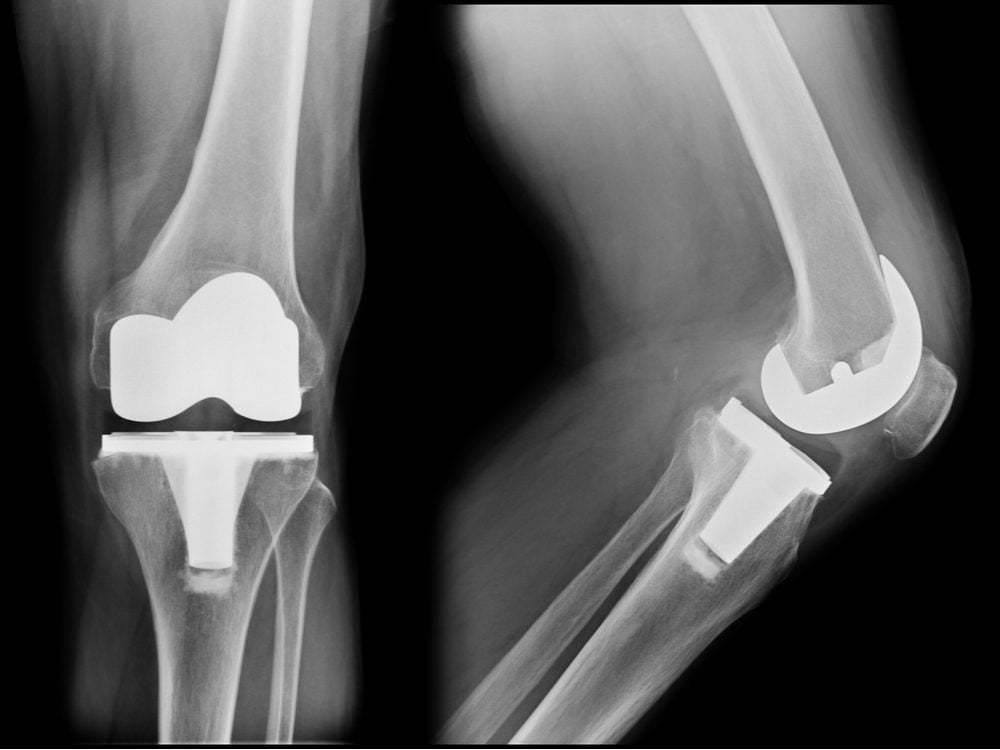
Put simply, an artificial knee works as a multidirectional hinge that connects the bottom of your femur (the upper leg bone) to the tibia (the shinbone). To install it, surgeons remove damaged cartilage and bone and connect the artificial knee to your bones. The surgery takes about an hour, involves a team of four to eight health care professionals supporting a lead surgeon, and is done with the patient under local or general anesthesia.
Doctors can choose from more than 150 sizes and variations of artificial knees. Most are made with polished titanium or a cobalt-chrome alloy, plus high-grade plastics, and can last for decades. For most patients, the type of implant is probably irrelevant, many experts say.
“The key is to trust that your surgeon is familiar with the device being used,” says Dr. Stephen Kelly, a joint-replacement surgeon at New England Orthopedic Surgeons in Springfield, Massachusetts. “Choose the surgeon, not the implant.”
Fill up on these anti-inflammatory foods that reduce pain.
When surgery isn’t the answer
Few would dispute that knee replacements are generally safe and, in most cases, appropriate. But not all doctors are convinced that replacement is the best answer for many patients.
One study looked at the level of patient-reported pain and knee function, along with X-ray evidence of arthritis, in people who got total knee-replacement surgery. The conclusion: About a third of the procedures were “inappropriate” using a standard classification system developed in Spain.
A 2015 follow-up study found that surgeries classified as inappropriate yielded little or no benefit in relieving pain or improving function. That is, patients with mildly bad knees had much less to gain from knee-replacement surgery than did those with severe pain or bone-on-bone arthritis.
“You don’t leap out of bed afterward,” says Dr. Nortin M. Hadler, who is emeritus professor of medicine at the University of North Carolina at Chapel Hill. “In addition to the inevitable risks of surgery, you have months of rehab ahead of you.”
Doctors wish you knew these facts about arthritis.
What to know before saying yes or no
Keep in mind these six concerns before you schedule your knee replacement.
1. There is no clear standard.
Surprisingly, there are no definitive criteria to determine whether you should undergo surgery, explains Daniel Riddle, a professor of physical therapy at Virginia Commonwealth University. Doctors assess three variables: pain, limits on daily activities, and visible evidence of bone damage. Only the last of the three can be measured objectively.
Ask your doctor to gauge how your symptoms compare with those of others, using a standardized scale that can be compared with research. The Knee Injury and Osteoarthritis Outcome Score is one example. “I’d want to know if my symptoms are considered mild, moderate, or severe, and what I can expect a year from now,” Riddle says.
2. Marketing is often inaccurate.
Surgeons likely will tell you that post-op, you should expect to dial back overall physical activity. But many hospitals promote surgery with ads showing fit people playing sports. Surgeons themselves can get caught up in the enthusiasm. “In professional meetings, there’s always someone showing pictures of patients surfing or mountain climbing,” says Dr. Kelly. “We all like to hold up our patients who are doing crazy activities.”
Dr. Hadler advises not even talking to a surgeon until you’ve had a thorough conversation with a primary care physician who has less of a stake in operating. And even if you are referred to a surgeon, keep an open mind. Most surgeons agree that knee replacement shouldn’t be taken lightly, even with its overall history of success.
“It’s major surgery,” says Dr. Joshua Jacobs, professor and chair of the Department of Orthopedic Surgery at Rush University Medical Center in Chicago. “You should contemplate it only after you’ve explored other options.”
3. Expectations vary.
In one European study, 93 per cent of patients were generally satisfied five years after surgery. But most also reported that they had expected more. Only one-third of those who considered sports or recreational activity important were pleased with their results.
And about 20 per cent of patients will have long-term pain, suggests one study review. Ralph Gabriel, now 73, is one of them. Post-surgery, he has been in constant pain, he says, and nothing he has tried so far—extensive physical therapy, electrical stimulation, over- the-counter painkillers—has helped.
Ask your surgeon detailed questions, specific to your hobbies and daily activities, about what you should and shouldn’t expect after the surgery. Most surgeons say you may have to forgo hobbies that require lateral movement and are high impact (such as singles tennis), because they could prematurely shorten implant life.
4. Recovery takes time.
“You have to work hard to get better from this operation,” Dr. Kelly says. That means six to eight weeks of rehabilitation and physical therapy to regain range of motion and rebuild muscles and ligaments that stabilize and support the knee.
Even with modern rehab techniques, one study found that a third of patients didn’t have measurable improvements in pain six months after surgery. Another found that one in eight patients still had moderate to severe pain one year post-op. In the latter study, however, almost all patients felt satisfied with their operations five years out.
Ask if your hospital has an education program that allows patients to meet with providers to understand what’s going to happen with their surgery and recovery. Dr. Kelly recommends that anxious patients also visit a physical therapist before surgery to discuss rehab.
All doctors are not the same.
Research suggests that you’ll do best with a surgeon who does more than 50 knee-replacement operations a year.
High- and low-volume surgeons had similar results on pain relief, one study found. But surgeons who do six or fewer knee replacements a year in low-volume hospitals may be less skilled at the soft tissue fine-tuning needed to achieve normal motion and full function. In that same study, patients of low-volume surgeons were twice as likely to score poorly on function measures such as being able to fully extend their knees two years after surgery.
Ask your surgeon about his or her outcomes, complication rates, infection rates and readmissions. Don’t settle for an answer from your surgeon citing national averages: You want his rate. The number should be around two per cent or lower.
Just as important, ask yourself whether your surgeon is taking a personal interest in what happens to you. A recent analysis of Medicare data [in the United States] by the independent journalism organization ProPublica found that surgeons with extremely low rates of complications tended to express a sense of personal responsibility for patients before, during, and after surgery.
5. Risks are small but serious.
The odds of having a major complication from knee-replacement surgery are relatively low. Few people assume they’ll be among the fraction of those who have more serious complications such as blood clots. “That’s why the discussion about risks needs to be more substantial than simply sign- ing a consent form,” Riddle says. “You need to have a detailed conversation with your doctor.”
The earlier you discuss possible complications with your physician, the better, Dr. Hadler says. “Once the mind-set is, ‘I need this,’ you don’t hear the risk, you hear the benefit,” he says.”
Here’s how the Cayman Islands are an increasingly popular option for Canadians seeking knee replacements.
The most common complications
While knee-replacement surgery usually goes well, complications do occur. Read on to learn which problems are most prevalent.
Failed implants: Prosthetics can pop out of the joint or wear down, releasing tiny particles of implant material. In osteolysis, particles trigger inflammation that can weaken bones and cause implants to come loose over time. About 10 per cent of joint replacements eventually fail and need to be redone.
Infections: An infection can be devastating, potentially destroying the function of the joint and, in the worst cases, threatening the patient’s leg or even life. Infections occur in only one to 2.5 per cent of cases, and doctors work to keep risks low with measures such as giving patients preventive antibiotics.
Blood clots: Clots are triggered by inflammation that occurs during healing—a process that boosts the risk of having a heart attack as much as 31 times for people 60 and older in the two weeks following surgery, according to a study in JAMA Archives of Internal Medicine. Knee patients routinely take blood thinners to reduce this risk.
Nerve injury: Nerves can be damaged as a result of complications of anesthesia, or the surgeon could damage a nerve during the operation. Both scenarios are rare, though, occurring in less than one per cent of cases. Nerve injuries can cause pain and numbness, but they generally improve over time, though not always.
Protect your joints by avoiding these arthritis trigger foods.
The newest technologies
Scientists are looking hard for better solutions that improve outcomes for knee-replacement surgery or bypass it with less invasive but equally successful procedures. Here are some of the options that have emerged.
Patient-Specific Instruments: Digital imaging creates tailor-made instruments that surgeons use just once to guide cuts and implant placement so they better match a patient’s anatomy and potentially preserve more of it. “It makes the operation shorter and more efficient,” says. Dr. Steven Haas, chief of knee service at the Hospital for Special Surgery in New York.
“Partial” Surgeries: Surgeons switch out just one part of the knee for an implant, leaving healthy cartilage, bone, and ligaments intact on the rest of the knee. Recovery tends to be quicker. “The trade-off is that partial knee replacements fall at a significantly higher rate than total knee replacements,” Dr. Haas says. Plus, there’s no guarantee you won’t have to come back for a total knee replacement if arthritis progresses. Only people with healthy ligaments are good candidates.
Robotic Surgery: Robotic systems can help surgeons position implants more precisely and consistently. “The surgeon controls the tool, and the robot keeps him from going outside the area he wants to cut,” says Jeremy Suggs, engineering manager at the ECRI Institute, a Philadelphia nonprofit that independently researches medical de- vices. Doctors most often use robotic systems for partial knee replacements that require extra precision to preserve ligaments.
Arthroscopic Procedures: People get “scoped” in a procedure called partial meniscectomy. It entails a surgeon go- ing into the knee through a “keyhole” incision, to trim and smooth jagged edges of torn meniscus, a layer of cartilage that cushions bones in the joint. Some studies, however, have found that this procedure produces no better results than sham surgery in which orthopedists scope the knee but don’t fix anything.
“That’s made a lot of surgeons pretty cautious about recommending arthroscopy for patients with arthritis of the knee,” says Dr. Craig Della Valle, an orthopedic surgeon and chief of adult reconstructive surgery at Rush University Medical Center.
Whether the balance of risk and reward finally steers you toward knee- replacement surgery depends on a lot of factors, but it ultimately comes down to your tolerance for one type of discomfort over another. “We tell patients, ‘You’ll know when you’re ready,'” Dr. Austin says. “They say, ‘What do you mean?’ Then they come back when they’re no longer willing to tolerate daily pain and dysfunction, and they say, ‘Now I understand.'”
Next, check out the latest news from the world of medicine.
Reprinted from the February-March 2017 issue of AARP The Magazine. © 2017 AARP. All rights reserved.