13 Silent Signs of Dementia (and How to Spot Them Early)
From sudden personality changes to poor financial decision-making, here are the 13 early signs of dementia you should never ignore.

Stephen Chow knew something was off when he started making more typos and spelling errors in his work emails. This was in 2010, and Chow, 51 at the time and living in Scarborough, was an IT specialist for Ontario’s Ministry of Government and Consumer Services.
He tried to ignore the mistakes at first, but the situation became more obvious when attempts to punch in his password kept failing. He found it gradually harder to focus and perform simple, familiar tasks, such as calculating numbers or putting his signature on a document. “Everything was all messed up, and I didn’t know what to do about it,” he says. Not wanting his wife, Eva, and two adult sons to worry, he kept it a secret from them, hoping he could just muddle through.
Instead, over the next several years, more alarming symptoms appeared. As Chow made the daily 90-minute drive to and from work, he had trouble seeing the centre line on the road, as well as the cars beside him. In early 2014, his patchy vision almost killed him when he couldn’t clearly discern the road’s edge and slid into the ditch during a snowstorm. He was unharmed, but his anxiety mounted, and he decided to talk to his family doctor.
When Chow described his difficulties with typing and driving—both related to motor skills—his physician initially referred him to a specialist in Parkinson’s disease. That condition was ruled out because he didn’t have hand or leg tremors. In May of 2014, Chow got an appointment with Dr. Carmela Tartaglia, a cognitive neurologist specializing in early-onset dementia at Toronto Western Hospital.
Tartaglia suspected Chow’s symptoms were visual-spatial processing problems, a warning sign of Alzheimer’s disease—and she noted one subtle but telltale clue. “Stephen’s writing difficulties became more apparent in Cantonese,” she says. “It’s his first language, and Cantonese is a more visual language than English.”
Weeks later, an MRI showed a shrinkage of cortical tissue in the back of his brain—the region involved in processing what and how we see—and biomarkers identified in his cerebrospinal fluid 18 months later finally confirmed, six years after Chow first noticed his symptoms, that he had early-onset Alzheimer’s disease.
Why detection of early dementia symptoms is key
Chow is one of about 700,000 Canadians living with dementia. Although the rate of people who develop dementia has been declining for decades due to healthier lifestyles, the total number is still projected to double over the next 15 years because of the aging population. Each year, more than 75,000 Canadians are diagnosed with some form of dementia. Around 10 percent are under the age of 65.
Detection of early dementia symptoms is important so that the person diagnosed, and their family members, can take steps to slow and mitigate the effects of the disease through lifestyle changes. Ideally, that would mean seeing a family doctor, undergoing specialized testing and receiving a formal diagnosis within six months or a year after noticing symptoms. But according to an Australian study, on average, it took two years for people to make an initial visit to a doctor and over three years for a firm diagnosis.
People often associate dementia with memory loss, but in many cases this is not the first sign. In fact, dementia can affect many different areas of the brain, and scientists now understand that symptoms differ based on where in the brain changes occur. With this knowledge, doctors now use advanced tools, such as brain scans and protein biomarkers, to make earlier, more specific dementia diagnoses.
But getting to that stage requires noticing that something is wrong—and letting somebody know.
“The first time I knew Steve had a problem was when he called me from Dr. Tartaglia’s office,” says Eva. Once the diagnosis was made, she realized there had been indications. She just wasn’t aware of what to look for.
Here are 13 early dementia symptoms that suggest you should be assessed.

Your personality changes
Inappropriate behaviour is an early symptom of damage to the brain’s frontal lobes, which regulate our social judgment.
“People with this dysfunction might undress in public, talk about people’s private parts or say ‘That person is stupid,’” explains Dr. Robin Hsiung, neurologist and associate professor at the UBC Hospital Clinic for Alzheimer Disease and Related Disorders. “They lose social graces and forget that what they’re saying or doing isn’t right.”
These symptoms are often seen in frontotemporal dementia (FTD), but also when Alzheimer’s or vascular dementia affect the frontal lobes. If they’re not recognized, they can be particularly unsettling.
“The worst symptoms for families to deal with are when there is a personality shift and the person becomes increasingly agitated or even paranoid and suspicious,” says Carrie Bourassa, a professor at the University of Saskatchewan’s college of medicine who specializes in dementia and aging in Indigenous populations.
Unusual behaviour can sometimes be confused with psychiatric conditions, such as bipolar disorder or schizophrenia, and brain imaging can help rule out or support a diagnosis of dementia.
You see things that aren’t there
Recurring visual hallucinations may be an early symptom of Lewy body or Parkinson’s disease dementia, although people with Alzheimer’s disease can experience them, too. These can be as simple as seeing flashing lights or as elaborate as encountering animals and people that aren’t real.
“Sometimes the hallucinations are quite frightening, like seeing a wolf or a bear trying to break through the window,” says Hsiung. “Other times they’re more positive, like a grandmother who looks out the window and sees her grandchildren playing in the playground, but no one is there.”
Researchers believe that visual hallucinations may be caused by damage to the brain’s visual-processing system, in combination with the disease’s disruption of the sleep cycle—so that the visions might actually be dreams breaking into waking consciousness.
You struggle with vocabulary
Word-finding difficulties are among the most common early dementia symptoms. You might have trouble finding the right words during conversations or when naming objects, sometimes substituting the wrong word. People affected in this way pause while speaking, use filler words and frequently rely on “it” or “they” instead of specific names for things. Researchers at the University of Wisconsin-Madison found that these word-finding problems increased significantly in the span of just two years for people developing dementia.
Language can, in fact, be affected before memory problems emerge. An Arizona State University study analyzed former U.S. President Ronald Reagan’s press conferences and found speech changes more than a decade before he was diagnosed with Alzheimer’s.
To assess whether your word-finding challenges are related to a shrinkage in the language areas of your brain, pay attention to when and how often this happens. It could simply be a result of being tired or stressed—and can be caused by anxiety, depression, stroke and delirium, as well.
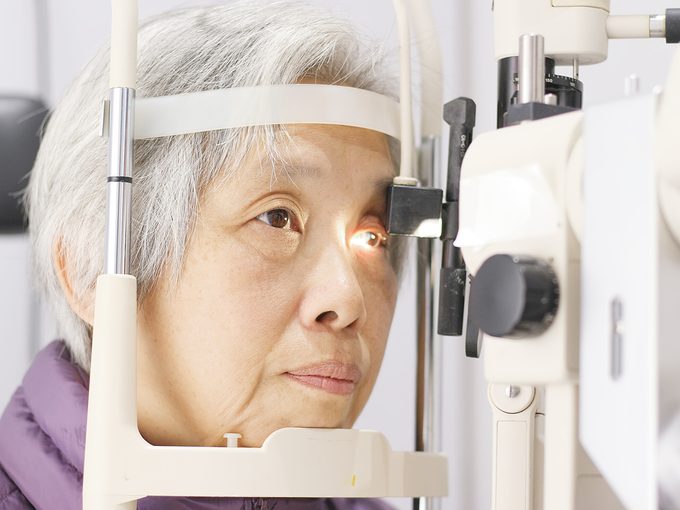
Your vision is patchy
Problems with spatial awareness can be caused by cataracts or glaucoma, but they’re also one of the early dementia symptoms. This was the case with Chow, whose first Alzheimer’s symptoms were caused by a shrinkage of the area of the brain crucial to his ability to accurately perceive the world three-dimensionally.
“A patient with posterior cortical atrophy may see the world in a patchy visual field,” explains Hsiung. “If the person is focusing in front while driving, he can’t see things off to the side. And if he’s changing lanes, he can’t see other cars beside him.” Meanwhile, when Chow made mistakes typing, he was having trouble seeing the whole keyboard.
Tartaglia notes that visual-spatial processing problems are especially prevalent as an early sign of Lewy body dementia, which can affect a similar area of the brain.
You find it difficult to keep focused
In addition to visual-spatial processing issues, Chow also had trouble with concentration due to shrinkage in his frontal lobe. “That made writing, reading and driving difficult and affected his ability to do high-level tasks as an IT specialist,” says Tartaglia.
Beyond Alzheimer’s, any other kind of dementia can affect this area of the brain—but note that an inability to focus can also be caused by anxiety, depression and side effects to medication.
You forget where you’ve put things
It’s not unusual to occasionally forget where you stashed your keys. But if you find that you’re doing this regularly, leaving the stove burner on or frequently forgetting recent events and conversations, this could be a warning sign. Commonly, says Hsiung, people with this type of memory loss will ask loved ones the same questions over and over again.
“Families can help a lot in recognizing these early symptoms, because if the person’s memory is poor, they won’t remember the problems they have in remembering,” he says.
This sign is one that often points to Alzheimer’s disease. In this type of dementia, the hippocampus—the brain area involved in forming, storing and retrieving memories—may be affected first. In fact, short-term memory loss is the most common symptom among people with Alzheimer’s disease, whereas it’s less often an early sign in vascular dementia and Lewy body dementia, and rarely in FTD.
Medications and depression can also affect memory, so it’s important to check with your doctor, who might recommend a screening test, such as the Montreal Cognitive Assessment—30 questions which quickly identify abnormal brain function.
You’re suddenly bad with money
A pattern of uncharacteristically poor financial decisions should set off alarm bells. “When you have frontal-lobe damage, you lose judgment and can make rash, impulsive financial decisions,” says Tartaglia. “A frugal person starts giving away more money or buying things they don’t need—like a furnace from a door-to-door salesperson.” She’s seen patients who did significant damage to their families’ finances, as well as CEOs of companies who lost millions because nobody noticed the signs.
A combination of declining decision-making skills and memory can also lead to financial lapses. A JAMA Internal Medicine study from 2020 found that people with dementia started missing bill payments up to six years before they were diagnosed.
You’re emotionally flat
According to a University of Cambridge study, a lack of interest or motivation can predict the onset of dementia many years before other cognitive symptoms do, especially in people with FTD, who may be diagnosed as early as age 45.
Hsiung cautions, however, that apathy can sometimes be confused with depression, as the difference between them is subtle; a psychiatric assessment is often required to tell them apart.
“In both, a person may sit on the sofa all day long,” he says, explaining that the key difference is how much their mood ranges. If someone becomes tearful when they hear a sad story, this could be depression, but it’s apathy if the person shows no emotional response. If it’s the latter, Hsiung says, it could be the beginning of Alzheimer’s disease, FTD or vascular dementia.
You’re not moving as well as usual
Difficulties with movement and performing physical activities in the right sequence can be an early sign of damage to the parietal lobe, which is related to motor skills—and this is one of the signs that Eva thinks she overlooked in her husband. Three years before his diagnosis, the couple began to participate in dragon-boat racing. Chow had always been a well-coordinated athlete and handyman, but during training he struggled to learn the basic stroke technique. “The coach kept telling him, ‘This is the way you do it.’ Steve didn’t get it very well, and he was upset with the coach,” says Eva.
Motor problems are also common with Lewy body dementia, but other neurodegenerative conditions, such as Parkinson’s and multiple sclerosis, should be considered, as well.
You’ve become insensitive
According to a 2016 Neuroscience Research Australia report, loss of empathy is a core symptom in some people diagnosed with FTD. It’s related to loss of grey matter in the social brain. These patients are unaware of the impact of their behaviour on others, and they lose both the ability to understand other people’s emotions and to share in their feelings.
“You may not care about your family anymore,” says Tartaglia. “Or a family member is crying, but you don’t recognize they are sad.”
You no longer grasp concepts you once did
Problems with tasks that require abstract thinking, such as understanding numbers or reading a house plan—especially if that was a strength before—are early dementia symptoms that can be caused by damage in the frontal and parietal lobes. For Chow, this appeared early at work in his inability to make simple calculations, but it also impeded his long-held role as the manager of his family’s finances. After his diagnosis, Eva took over those duties.
You’re more anxious
Mood changes, such as depression and anxiety, can be early dementia symptoms that start well before people begin to experience memory loss, according to a 2015 Neurology study. Tartaglia notes that, especially with Lewy body dementia, non-anxious people can become anxious much of the time. They may exhibit persistent worry, fear or agitation, commonly triggered by going outside the home or being separated from a family member.
You get lost more often
Losing navigational skills, and the ability to create a mental map of your environment, can be one of the early dementia symptoms. In fact, in 2019, University of Cambridge researchers developed a virtual-reality navigation test that has proven to be better at identifying early Alzheimer’s disease than FDA-approved neuropsychological tests currently considered to be a gold standard for early diagnosis.
“We built a running track in our backyard so Steve could jog safely every day without getting lost,” says Eva.
Once Chow was properly diagnosed, his anxiety about his symptoms decreased and he became calmer. “Eva is the model caregiver because she wants to do what’s best for Stephen and encourages him to do things,” says Tartaglia. This has included joining Alzheimer Society of Toronto programs and support groups for people with early-onset dementia, practising daily meditation and getting regular aerobic exercise.
But perhaps most importantly, with Eva’s encouragement, Chow began to share his dementia diagnosis with the people in his life. “I felt better after I told my family and friends,” he says. “They were very supportive, and it took a load off my shoulders. I learned that you should tell people what you’re noticing sooner rather than later and not keep it to yourself.”
Types of dementia
Rather than one specific disease, dementia describes a group of symptoms that are caused by disorders affecting the brain. There are more than a dozen types of dementia, including rare conditions and others that may develop from other brain disorders, like Parkinson’s disease or Huntington’s disease.
Here are the five most diagnosed forms of dementia:
Alzheimer’s disease is the most common type of dementia, accounting for up to 80 percent of all diagnoses. Generally, Alzheimer’s affects most areas of the brain as it progresses and can therefore involve changes in memory, language, problem solving, mood and behaviour.
Vascular dementia, the second-most-common type, happens when there is a blockage to the brain’s blood supply, which causes brain cells to be deprived of oxygen and die. Strokes, transient ischemic attacks and blood-vessel disease are common causes of vascular dementia and can affect different brain areas.
Lewy body dementia is caused by abnormal deposits of a protein called alpha-synuclein inside the brain’s nerve cells. This protein, which destroys brain cells, is also found in people with Parkinson’s disease. Areas of the brain involved in thinking, movement and visual processing are most affected.
Frontotemporal dementia mainly affects the frontal and temporal brain areas and accounts for about 20 percent of cases of early-onset dementia. Changes in personality and behaviour are more apparent in the early stage, while memory decline often doesn’t occur until later.
Mixed dementia occurs when a person has at least two different types of dementia, most often Alzheimer’s disease and vascular dementia. Studies reveal it’s much more common than previously thought.
Now that you know how to spot the early dementia symptoms, find out how this MIND diet meal plan feeds your brain.







