
Using Medical Marijuana to Treat Illnesses
About 15 years ago, James O’Hara began experiencing an aching pain and stiffness in his left hip, symptoms that were eventually diagnosed as osteoarthritis. The former banking executive, now 60, managed the condition with Tylenol and Advil for a while, before finally turning to a prescription drug. After a few years, one of the medication’s side effects—stomach upset—became so severe that it caused what’s known as refractory pain, which travelled up a nerve to O’Hara’s left ear. “It was horrific,” he says, and for years he relied on an ever-changing cocktail of prescription medications to combat the side effects from the first one, with varying levels of success.
The idea of trying cannabis as an alternative came to O’Hara five years ago, after several of his friends began using it for their own health problems. Despite not having smoked pot regularly since his early 20s, O’Hara experimented with recreational marijuana for pain control and eventually got a formal prescription from a cannabis clinic.
“I was shocked at how well it worked,” says O’Hara, who this March became CEO and president of Canadians for Fair Access to Medical Marijuana. “With it, I could function better, and mentally, I was a lot clearer.”
As well as suffering from osteoarthritis, O’Hara experiences focal seizures as a result of an old head trauma, which make him forgetful and disoriented. Since beginning to take medical marijuana, he says these seizures have been reduced by about 85 per cent. On top of that, he believes cannabis helps his chronic asthma.
“I was surprised by these unexpected benefits,” he says. “For me to realize I had gone through my life not knowing that this was available to me made me quite angry. It made me ask, ‘Why aren’t we talking about this more?’”

The Grey Areas of Medical Marijuana
Approximately 292,000 Canadians are registered users of medical marijuana. Many of those who have tried it are enthusiastic about its benefits, but doctors and researchers point out that we still don’t have enough data to be confident that it’s as effective as some believe. Fortunately, evidence from studies—most of which employ cannabinoids, the chemical compounds present in the cannabis plant—is beginning to get clearer around a number of different uses.
For many disorders, there’s not enough information to conclude whether marijuana is beneficial, mainly because there haven’t been enough high-quality clinical trials—the kind required before a pharmaceutical drug is allowed into the marketplace for use.
According to Fiona Clement, an associate professor at the University of Calgary, the lack of research is primarily due to the fact that medical marijuana has only been allowed for use since 2001 and has been subject to a more stringent approval process from Health Canada in order to study it. “And there’s also an issue of funding,” she says. “Historically, this has been an illegal industry that’s not in a position to support research.”
One interesting area of debate is anxiety. We know that people with anxiety disorders are more likely to use marijuana, but it’s unclear whether the plant helps control their anxiety or contributes to its development.
“People report that they take it to relax, so it’s natural to conclude that cannabis might help with anxiety,” says Ziva Cooper, an associate professor at Columbia University. However, we are still awaiting proper clinical trials to prove it.
Don’t miss the accidental history of 10 common drugs.
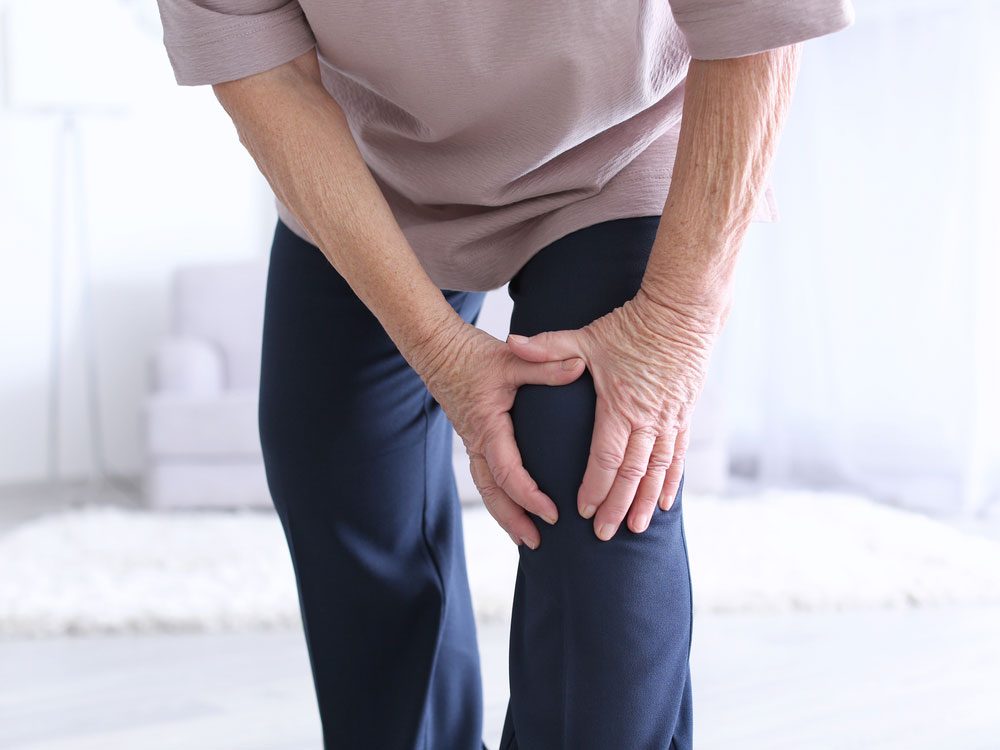
Where the Evidence is Strong: Chronic Pain
In 2013, 65 per cent of Canadians using medical cannabis were prescribed it for pain related to severe arthritis. Pain relief in general is what often motivates people to try it for the first time. With more than 30 randomized controlled trials on using cannabinoids for this purpose, it’s also one of the best-researched areas. The results have been contradictory, with some studies concluding that cannabis or cannabinoids work for pain, and others finding they are no better than a placebo. But more and more doctors are giving them a thumbs-up.
“[The effectiveness of cannabis] isn’t proven yet, but the evidence is growing,” says Andrea Furlan, senior scientist at the University of Toronto faculty of medicine and co-chair of Project ECHO Ontario, which helps primary care providers choose the best treatments for chronic pain. Although Furlan notes that we still need larger studies and ones that look at a wider range of conditions, she says it’s reasonable for people to turn to prescription cannabis for pain, especially if other treatments aren’t working.
Scientists are still unsure exactly how marijuana might work to combat pain. Cannabis affects the endocannabinoid system—receptors in the brain that are connected to appetite, pain, mood and memory—but we don’t know what those receptors do. However, in addition to interacting with the physical aspect of pain, it seems that marijuana may ease its psychological side, as well.
“Pain is the alarm system in our body, so it activates the emotional part of the brain,” explains Furlan. “It makes you feel like you cannot wait, that you have to stop everything you’re doing and fix it.” For chronic pain, she says, that reaction isn’t useful, because there’s nothing to fix. Patients tell her that cannabis helps dull those strong emotions.
Try these 11 pain management strategies for everyday aches and pains.

Where the Evidence is Strong: Multiple Sclerosis
Canada has one of the highest rates of MS in the world, with over 90,000 of us living with the condition. Cannabinoids seem to help sufferers with one of the disease’s core symptoms, spasticity—stiffness that can make movement difficult and cause painful muscle spasms.
Studies examining assessments by doctors tend to find improvements so small they could be due to chance, but reports from patients have been more positive. One 2012 study, run by 22 institutions in the U.K., found that 29 per cent of patients who took a cannabis extract said their symptoms had improved, while only 16 per cent of those taking a placebo reported a positive effect. That adds up to “substantial evidence that cannabis can help improve patient-reported spasticity,” says Ziva Cooper, one of the co-authors on a National Academies of Sciences, Engineering and Medicine report on cannabis and cannabinoids.
Be aware of these 11 diseases doctors are most likely to miss.
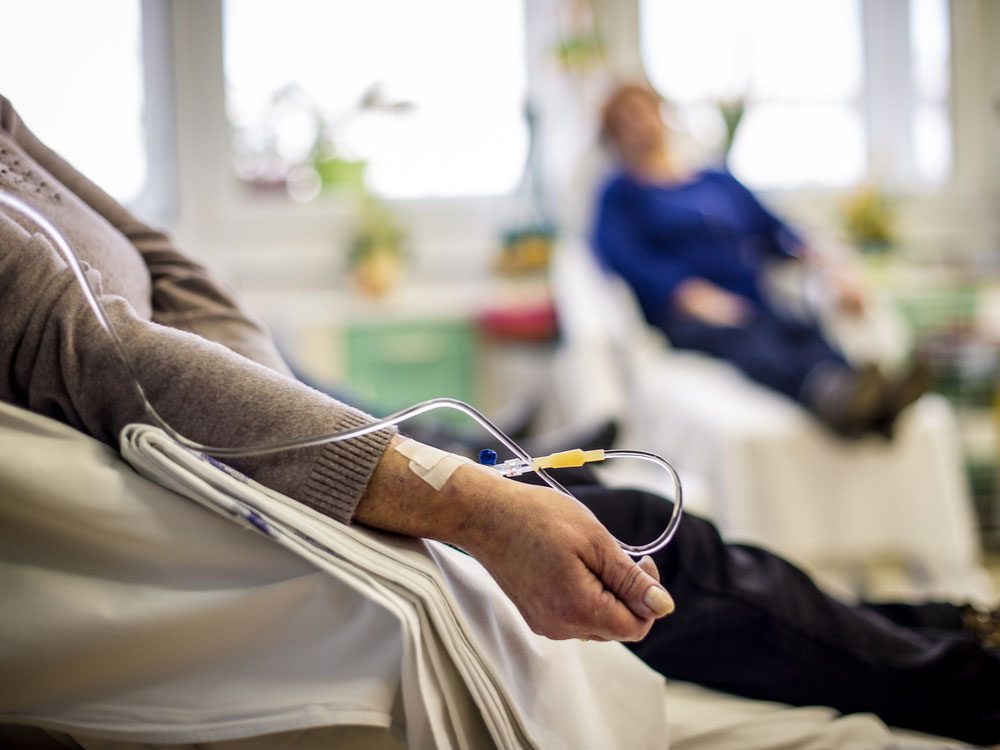
Where the Evidence is Strong: Nausea from Chemotherapy
The interaction between cannabis and chemotherapy is another area that’s well studied. In 2015, the Cochrane Collaboration—an international non-profit that analyzes evidence around health interventions—concluded that people undergoing chemotherapy who took cannabinoids were three times less likely to experience nausea and five times less likely to have that turn into vomiting than those who had been given a placebo. In fact, those positive findings mean that, for some patients, medical marijuana could be just as effective as the traditional anti-nausea drugs currently prescribed.
The Cochrane Collaboration did warn, however, that patients reported more side effects from cannabis-based medications than with conventional ones, including feeling high, dizzy or sedated. Shelita Dattani, director of practice development and knowledge translation for the Canadian Pharmacists Association, says that’s why it’s not doctors’ first choice for nausea. “It’s adjunctive therapy,” she says. “It would be used for patients who have not responded to the multitude of traditional options out there.”
Here’s how magic mushrooms may help people with terminal cancer.

Where the Evidence is Strong: Insomnia
People frequently turn to marijuana to help with sleep problems, and there is promising evidence that cannabinoid-based medications can work for them.
So far, most of the research has looked at marijuana’s effectiveness when it comes to improving sleep disturbed by medical issues like sleep apnea, fibromyalgia or MS. Cannabis seems to improve both how much sleep people get and how restorative it is, with many patients reporting less daytime fatigue.
Although researchers are unsure why it has this benefit, some hypothesize that the tetrahydrocannabinol (THC) in marijuana—the compound that makes you feel high—acts as a sedative.
Follow these tips on how to fall asleep fast with natural sleep aids.
Where the Evidence is Strong: Epilepsy
Marijuana’s ability to stop seizures became famous in part thanks to a 2013 CNN documentary, Weed, featuring a child—Charlotte Figi—who had hundreds of seizures a week, which robbed her of the ability to walk, talk and eat. When Figi was five, her parents persuaded doctors to prescribe her cannabis oil, and the frequency of Figi’s seizures dropped to two to three times a month.
Those kinds of “profound case reports” inspired more rigorous research on the effects of cannabinoids, especially in children, says Fiona Clement, an associate professor at the University of Calgary. A recent study on cannabinoid use for children with treatment-resistant epilepsy conditions reported the frequency of seizures dropping by upwards of 20 per cent—and sometimes down to zero.
These 100+ health studies will change the way you live.
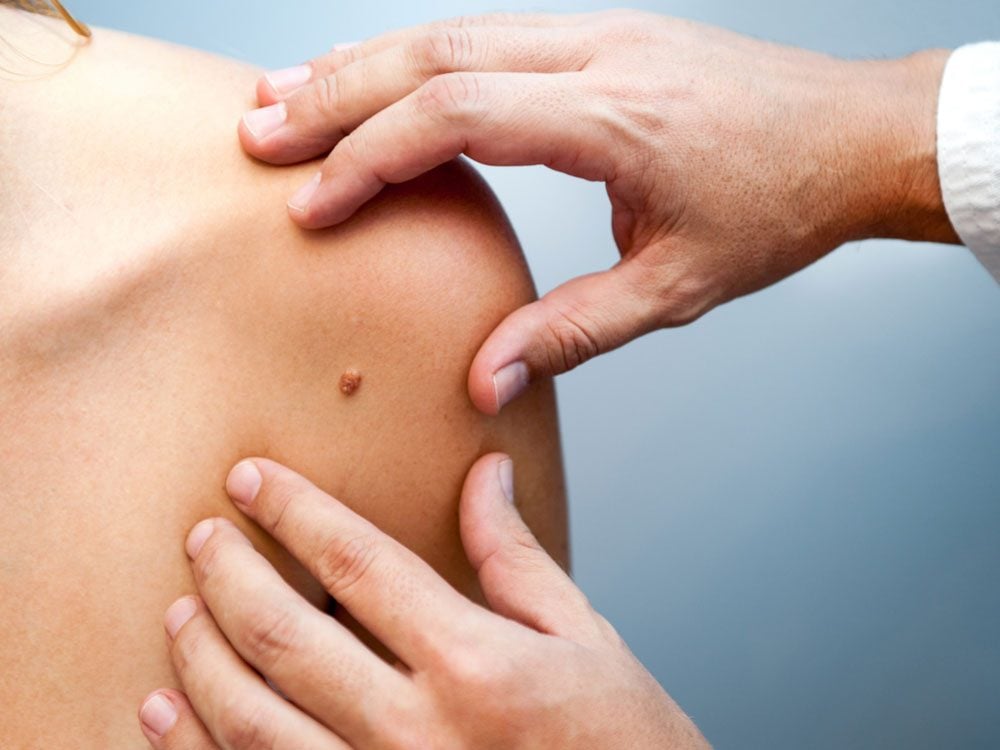
Where the Evidence is Weak: Cancer
Stories have long swirled on the Internet that marijuana cures cancer; some unscrupulous doctors have even built their practices around this idea. Cannabinoids have been shown to kill cancer cells in the laboratory, but that’s a long way from curing cancer in real life—in other studies, researchers found that cannabis also harms crucial blood vessels, weakens the immune system or even encourages some cancer cells to grow. The evidence of its effectiveness in people with cancer is mostly anecdotes about patients making miraculous recoveries, which could be coincidental.
So far, there have only been a few very small clinical trials in this area. One found a positive effect with adding cannabis to standard chemotherapy—but was observed in a sample of only nine people with aggressive brain tumours. “I’m not a believer,” says Clement. “Cannabis doesn’t cure cancer.”
Meet the dogs that can sniff out cancer.

Where the Evidence is Weak: Dementia
Some studies have found that cannabinoids help remove amyloid clumps—the protein buildup in the brain that is a hallmark of Alzheimer’s disease—in lab mice, and increases their ability to learn. However, human trials haven’t yet been run, and it’s not unusual for drugs to benefit animals and fail in people.
In the meantime, other research has shown that heavy marijuana users score worse on cognitive tests while high, with diminished memory and attention, suggesting that there is still a lot to learn about how medical marijuana could affect our mental abilities.
Learn how to prevent dementia with these 50 everyday habits.

Where the Evidence is Weak: Glaucoma
The belief that marijuana helps treat glaucoma started in the 1970s, when studies showed that it lowered pressure in the eyes—one of the condition’s causes, which can lead to vision loss. However, follow-up studies found that marijuana only maintained this result for a few hours, so sufferers would have to use the drug up to eight times a day for it to be beneficial.
Cannabis also reduces blood flow to the optic nerve, which can damage it and cancel out any positive effects of lowered pressure. Newer prescription medications, on the other hand, work for much longer without those issues, so doctors recommend them over medical marijuana.
Beware of these silent signs you might have eye cataracts.

Choose the Right Strain for You
Medical marijuana comes in hundreds of strains with many different components, but the two we know the most about are tetrahydrocannabinol (THC)—which produces the euphoria we associate with pot—and cannabidiol (CBD), the part that seems to be behind most of the known medicinal effects. Many people who are prescribed the drug opt for strains high in CBD and low in THC to get the health benefits without the high.
Here’s what you need to know to determine if telehealth is right for you.

The Dangers of Using Medical Marijuana
Doctors warn against smoking cannabis, as that can cause breathing problems and might be carcinogenic; a vaporizer, which boils the buds rather than burning them, reduces those issues. Edible versions and oils don’t have that problem, but it’s difficult to estimate proper dosages with them. For these, it’s important to start with a small quantity and wait at least two hours before having more. Cannabinoids are also available as brand-name drugs for some medical issues, making it easier to find the right type and dose.
Shelita Dattani, an Ottawa-based pharmacist, notes that there’s a misconception that marijuana is innocuous; like any drug, it has side effects. The most common are dizziness, dry mouth, nausea, fatigue, drowsiness and euphoria. That’s another reason why doctors suggest you “start low and go slow.” Additionally, cannabis can interact with other medications, so be sure to tell your doctor that you’re using it, if they’re not already aware.
Next, check out what happened when one woman tried CBD to treat anxiety, chronic pain and stress.