
A Life-Saving Treatment for Diabetes
A diabetes diagnosis used to mean certain death. Before the 1900s, the only treatment was an extreme diet, which slowed the progression but never stopped the decline caused by the disease. In 1897, the average life expectancy of a 10-year-old diagnosed with diabetes was one year. At the age of 30, it was four years. And for someone diagnosed at the age of 50, they were expected to live less than eight years. But in 1921, two doctors at the University of Toronto, Dr. Frederick Banting and Dr. Charles H. Best, began experimenting and made a life-saving discovery—a drug called insulin. While not a cure, the discovery dramatically added years to the lives of millions of people living with the disease. The pair won the Nobel Prize in 1923.
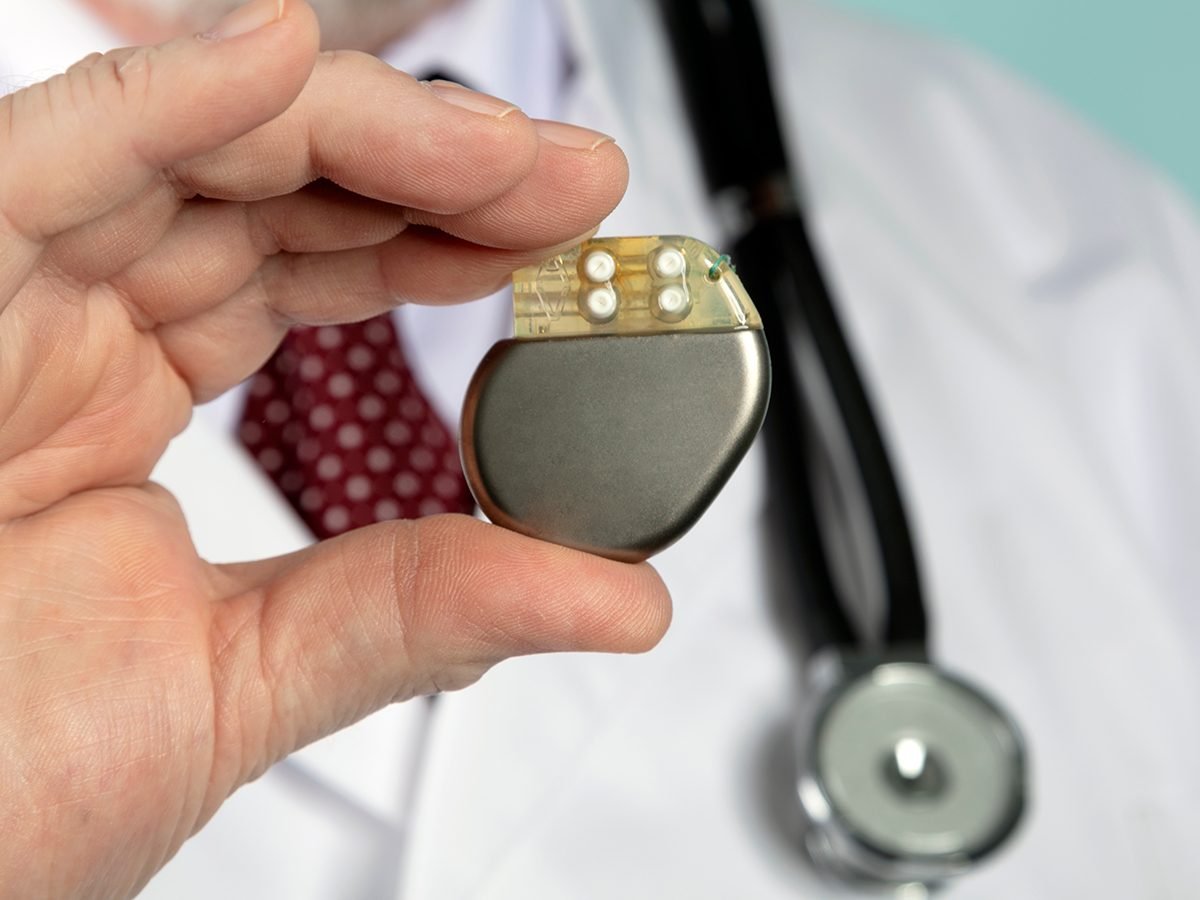
The Invention of the First Pacemaker
In 1949, Dr. John Hopps, in collaboration with researchers at the University of Toronto Banting Institute, developed the world’s first cardiac pacemaker. His discovery led to the development of implantable versions using transvenous catheter electrodes, which Dr. Hopps also developed. Cardiac pacemakers are life-saving devices used around the world to help control heart rhythms.
Here are 50 heart health tips cardiologists wish you knew.

Uncovering a Main Cause of Infertility
In the 1960s, Dr. Henry Friesen, an endocrinologist at McGill University, discovered the human pituitary hormone called prolactin. This helped to uncover its role in infertility, and Dr. Friesen developed a blood test, which allowed thousands of people with prolactin-related reproductive disorders to have children. Dr. Friesen’s research around prolactin helped to develop the drug Bromocriptine, which is used to treat female infertility around the world.
Did you know that doing this everyday could lower your fertility?

The Discovery of the Cystic Fibrosis Gene
In the 1980s, cystic fibrosis (CF), a genetic disease that affects the lungs and digestive system, was a fatal diagnosis. The average life expectancy was around 20 years in Canada, and even lower in many countries around the world. In 1989, doctors at The Hospital for Sick Children, Dr. Lap-Chee Tsui, Dr.Manuel Buchwald and Jack Riordan discovered the gene that causes CF. Dr. Tsui was inducted into the Canadian Medical Hall of Fame for “the most significant breakthrough in human genetics in 50 years.” This discovery was the first step towards a cure for thousands of affected patients and has led to many further discoveries about the origins of this hereditary and devastating disease.
Check out the 40+ health news stories you need to read this week.

Using Stem Cells to Stop Cancer
Canadians have always been leaders in stem cell research. In 1994, Toronto physician Dr. John Dick isolated cancer stem cells, to find that colon cancer originates from a rare type of colon cancer stem cell. His research lay the groundwork for the development of treatments that target and destroy cells that cause cancer. He also uncovered isolated human leukemia stem cells that can cause leukemia to develop. In 2010, a team of researchers in Hamilton, led by Dr. Mick Bhatia, discovered important differences between abnormal cancer cells and healthy human embryonic stem cells – the first in the world to make this discovery which could lead to more targeted cancer treatments.
Here are 6 silent signs of colon cancer symptoms to look out for.
Performing Ground-Breaking Transplants
Canada has a long history of innovation when it comes to life-saving transplant discoveries. In January 2017, doctors saved a woman’s life by removing her infected lungs prior to an available transplant, a medical first. She survived the procedure and received a successful lung transplant six days later. In 1988, the first successful liver-bowel transplant worldwide was performed in London, Ontario. And in the 1950s, doctors in Toronto performed the world’s first successful transplant of heart valves. Canadian physicians have also made major advances in fetal heart interventions, saving the lives of children before they are born. And doctors in Toronto completed the nation’s first successful hand transplant in January 2016.
Read the heart-warming story of how one woman’s life was saved when her cousin gave her a kidney.
The First Ebola Vaccine
The largest epidemic of the Ebola virus ravaged West Africa in 2014 and 2015, causing more than 11,300 deaths. Thanks to Canadian researchers, future Ebola outbreaks could be prevented. A Canadian-developed Ebola vaccine, partially designed by researchers at Canada’s National Microbiology Laboratory in Winnipeg, was found to be highly protective in a major clinical trial in Guinea. The vaccine trial signaled a 100-percent protection rate for more than 5,000 people who were vaccinated.
Here’s what you need to know about the new COVID-19 vaccines.

The Discovery of an ALS Gene Mutation
You may recall the Ice Bucket Challenge, which went viral online in 2014. But what you might not know was that it helped support amyotrophic lateral sclerosis (ALS), a devastating neurodegenerative disease which leads to a loss of mobility and eventually death. And Canadians have played a big part in finding the origins of this disease. In 2013, Dr. Michael Strong and his research team at Western University in London, Ontario, discovered a new gene that causes ALS. Finding out which mutant genes create abnormal proteins is important for scientists to develop new treatment options.
Discover the latest medical news that could save your life.

Surgery Goes Social
In 2014, Sunnybrook Health Sciences Centre in Toronto made medical history by live tweeting a heart bypass surgery. During the operation, the team shared pictures and answered questions. The aim was to raise awareness about cardiac disease during February’s Heart Month. Since then, Sunnybrook and Toronto East General Hospital have used the power of social media to live tweet colon cancer and prostate cancer surgeries, raising awareness about the importance of screening and men’s health.
Learn about how this doctor helps breast cancer patients prepare for treatment.

Using Viruses to Kill Cancer Cells
In 2015, Canadian researchers launched the world’s first clinical trial of a therapy that uses a combination of two viruses to stimulate an anti-cancer immune response and subsequently kill cancer cells. Immunotherapy has great potential, not only to cure cancer, but also because it has less harsh side effects than conventional radiation and chemotherapy treatment. Scientists in Ottawa are currently working on ways to engineer patient’s T-cells (which are involved in immune response) and are launching human clinical trials. That means more therapies could become widely available.
Next, here are the 60 most important inventions from the year you were born.