
What the CT scan uncovered
The patient: Gavin, a 43-year-old Holstein cattle farmer
The symptoms: Compressed abdomen, vomiting
The doctor: Dr. Stuart Whitelaw, consultant surgeon, Dumfries and Galloway Royal Infirmary, Scotland
Ten years ago, on a frosty December morning, Gavin was attempting to deliver a breech calf in a field on his small farm in southwest Scotland. The birth took hours and when it was finally over, Gavin collapsed on the ground—and the exhausted cow collapsed on top of him. Gavin’s cries for help were eventually heard by a neighbouring farmer, who attached ropes to his tractor to pull the animal away. Gavin was conscious but in severe pain. He was transported by helicopter to Dumfries infirmary, 120 kilometres away.
He had bruising over his ribs and abdomen, but no bones appeared to be broken, his blood pressure was normal and he was lucid enough to answer questions. After 12 hours of observation, the farmer was worried about his livestock and asked to go home, but doctors convinced him to remain overnight. The next morning, he began vomiting large amounts of greenish, small-bowel fluid. Doctors ordered a second CT scan and discovered a complete obstruction in his small bowel that hadn’t been visible before.
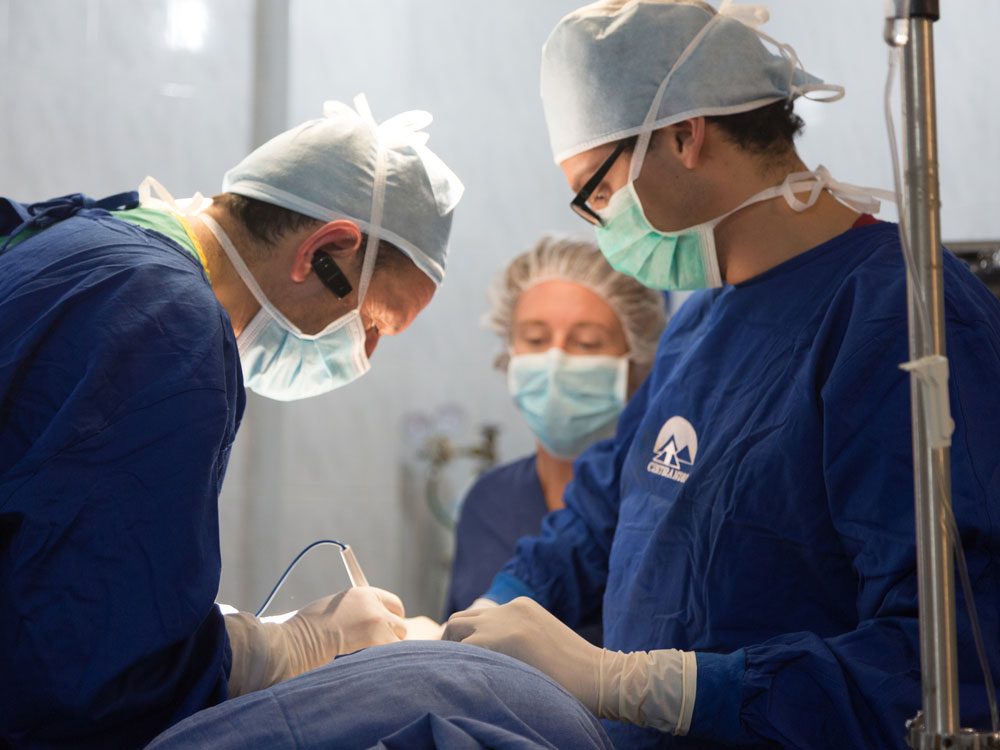
A frightening discovery
An exploratory abdominal operation revealed that a loop of the bowel was trapped by an adhesion, a band of scar tissue that binds two other tissues together that are not normally attached. Ninety per cent of these occur after abdominal surgery, says Dr. Stuart Whitelaw, but they can also be the result of an injury. “It’s likely in this case that the patient suffered a long-forgotten blow to his abdomen in childhood (perhaps falling from a tree or receiving a punch on the playground) that led to the development of an adhesion.”
Had the cow not fallen on Gavin, the abdominal adhesion may never have caused a problem, Whitelaw says. “But the cow compressed his abdomen and, bizarrely, forced the intestine through a gap caused by the adhesion.” It was a life-threatening problem. The small bowel would become strangulated, blood flow would stop and the integrity of the lining of the bowel would be compromised. This could allow bacteria into the bloodstream, leading to septic shock and multiple organ failure. That same result could occur if a perforated bowel allows bacteria to leak into the nearby abdominal cavity.
Whitelaw performed an emergency operation to divide the adhesion and relieve the obstruction, but while he was inspecting Gavin’s other organs, he noticed a small tumour on the patient’s cecum (a pouch at the beginning of the large bowel). The doctor removed the tumour by cutting out the right side of the large bowel. He then joined the ends together and sent the specimen to the lab. Gavin, meanwhile, made a quick recovery and within days was back on his farm, attending to the new calf and its mother.
These are the cancer symptoms you should never ignore.
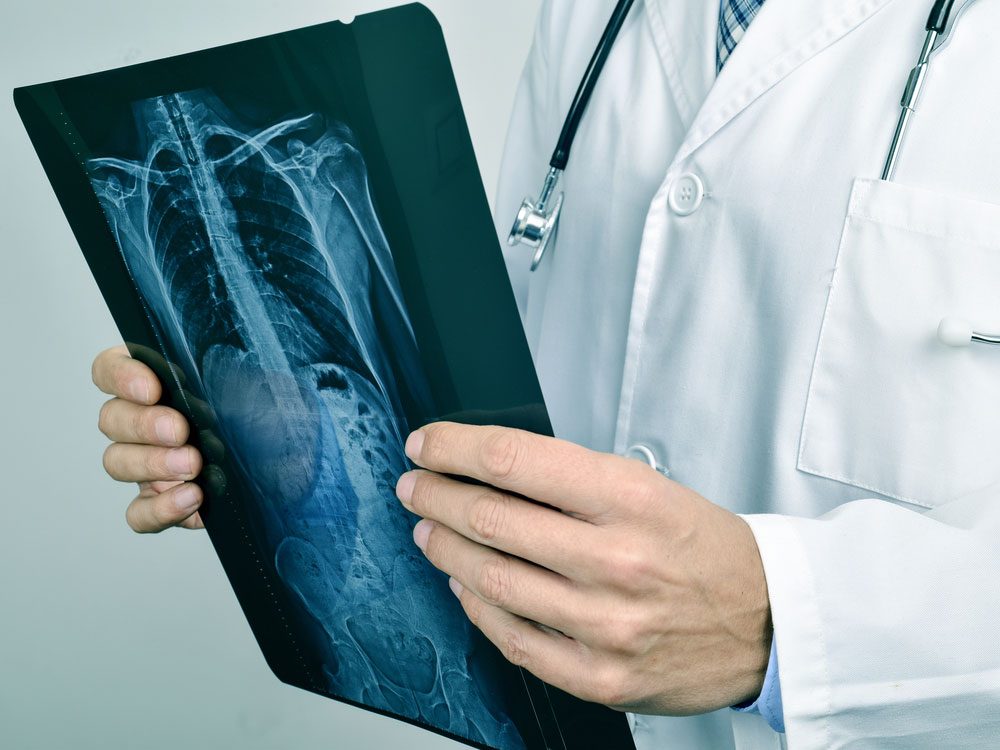
“The farmer saved the cow and the cow saved the farmer.”
A week later, the pathology report revealed that Gavin had early-stage bowel cancer, caused by a genetic mutation. Fortunately, it had been caught early. “When removed at this stage, the prognosis is very good, with a 95 per cent five-year survival rate,” Whitelaw says. Often patients with bowel cancer don’t have any symptoms or, by the time they manifest, it’s too late because the tumour is more advanced. “If the cow hadn’t fallen on him, his diagnosis would have been delayed, the tumour would have grown and he might have presented at a later stage when the prospect of a cure was less likely, or even impossible.”
A decade later, Gavin continues to do well, and the cancer shows no sign of recurrence. And, thanks to his diagnosis, his three children can have DNA testing to see if they also carry the cancer gene and require further screening, Whitelaw says. “In the end, the farmer saved the cow and the cow saved the farmer—and potentially his children and their children.”
Here’s how to tell which cancer screenings you really need.